Medical credentialing is vital for ensuring that healthcare professionals are qualified to provide high-quality care and minimize malpractice risks. This process involves verifying a healthcare professional’s education, training, licensure, board certifications, and work history. It is a critical step in healthcare credentialing that ensures the safety and efficacy of medical care.
To participate in Medicare, healthcare providers must have an NPI number and complete an application that includes information about their credentials, licensure, and experience. Additionally, healthcare providers must be registered with their state Medicaid agency and meet specific state credentialing requirements to join the Medicaid program.
Given the complexity of the credentialing process for providers, it’s essential to adopt efficient practices. Here are seven steps to help improve the medical credentialing process, making it less time-consuming and more effective:
7 Steps to Improve the Medical Credentialing Process
Credentialing in healthcare can be time-consuming and frustrating. To streamline the provider credentialing process and improve efficiency, follow these seven steps carefully:
1. Identify the Required Credentials
Understanding and identifying the necessary credentials is crucial in ensuring healthcare professionals meet the qualifications for their roles. This process involves determining the specific education, training, licensure, and other requirements needed to practice in your healthcare organization.
Common qualifications and credentials include:
- Education: Degrees from accredited medical schools
- Training: Completion of residency programs
- Licensure: State medical licenses
- Board Certifications: Certification in relevant specialties
- Work History: Previous employment verification
Ensuring these credentials are accurately identified helps maintain the high standards of care within your organization.
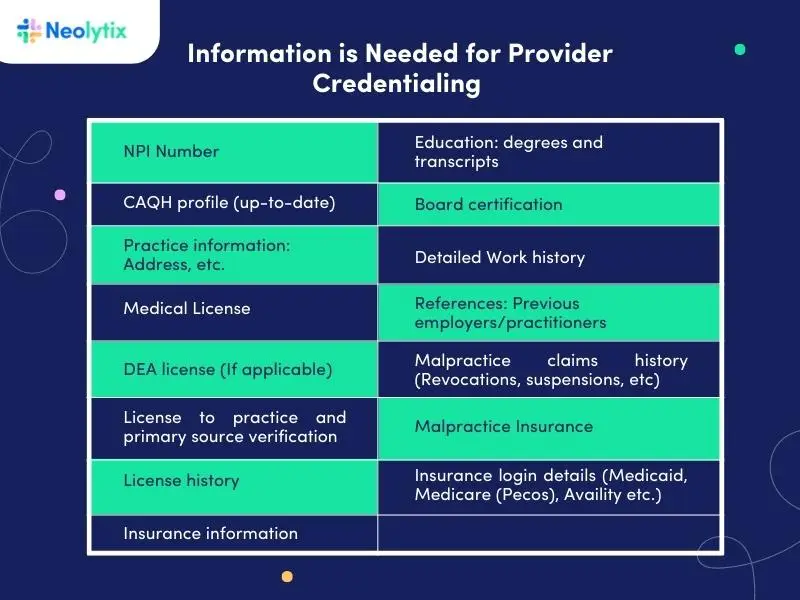
2. Gather Necessary Information
Collect all required documentation and verify the healthcare professional’s work history, licensure, education, and board certifications. Having complete and accurate information is essential for a successful credentialing process in healthcare.
3. Verify Primary Sources
Checking primary sources is crucial for verifying the accuracy and reliability of a healthcare professional’s information during credentialing. It involves obtaining information directly from primary sources such as licensing boards, medical schools, and previous employers.
4. Use a Centralized System
A centralized system for the medical credentialing process ensures all necessary documents are received on time and deadlines are met. It provides a streamlined approach to managing the entire process and allows for efficient communication between all parties involved.
5. Adopting Technology
Incorporating technology can automate parts of the credentialing process, reducing the time required. Electronic verification of licensure and board certifications, for example, can significantly speed up the provider credentialing process steps.
6. Prioritize the Process
Giving the credentialing process the necessary attention and resources ensures it is not delayed by competing priorities. Prioritizing the process helps it be completed promptly and efficiently.
7. Follow Up Regularly
Regular follow-ups with healthcare providers and relevant parties are crucial for maintaining smooth communication and addressing any issues quickly. This step is often overlooked, leading to delays in the credentialing workflow. Additionally, regular check-ins are important for communication. They help resolve issues quickly and keep the process on track.
For many healthcare organizations, this step is the biggest culprit when it comes to delays. Office workers are too busy with their tasks. They cannot also be responsible for scheduling and conducting regular check-ups like police officers.
Read More: Credentialing 101 Guide for Therapists
Overcoming Common Credentialing Issues in Healthcare
The credentialing process for providers is crucial for maintaining high standards in medical care. Addressing common credentialing issues in healthcare can streamline the process and ensure healthcare professionals are properly vetted.
Credentialing in Medical Billing
Ensuring accurate documentation is vital in the credentialing process in medical billing. This impacts the provider’s ability to offer services and affects reimbursement. Utilizing technology and a centralized system can expedite provider credentialing in medical billing, reducing errors and delays.
Types of Credentialing in Healthcare
There are various types of credentialing in healthcare, tailored to different roles. This includes credentialing for physicians, nurses, allied health professionals, and medical assistants. Understanding specific provider credentialing requirements for each role ensures comprehensive credentialing.
The following types of credentialing are essential for ensuring that healthcare providers are qualified and competent, ultimately protecting patient safety and maintaining high standards of care.
- Primary Source Verification (PSV): This involves directly verifying a practitioner’s credentials with the issuing institutions, such as medical schools, residency programs, and licensing boards.
- Hospital Privileging: This process grants practitioners the authority to perform specific procedures and services within a hospital. It involves a thorough review of the practitioner’s qualifications, experience, and competency.
- Board Certification: This is a voluntary process where physicians demonstrate their expertise in a specific medical specialty by passing rigorous exams and fulfilling continuing education requirements.
- State Licensing: Each state requires healthcare providers to obtain a license to practice. This process includes verifying education, training, and passing relevant exams.
- Health Plan Credentialing: Health insurance companies conduct this type of credentialing to ensure providers meet their standards before being included in their network. It involves verifying qualifications, reviewing malpractice history, and assessing overall competency.
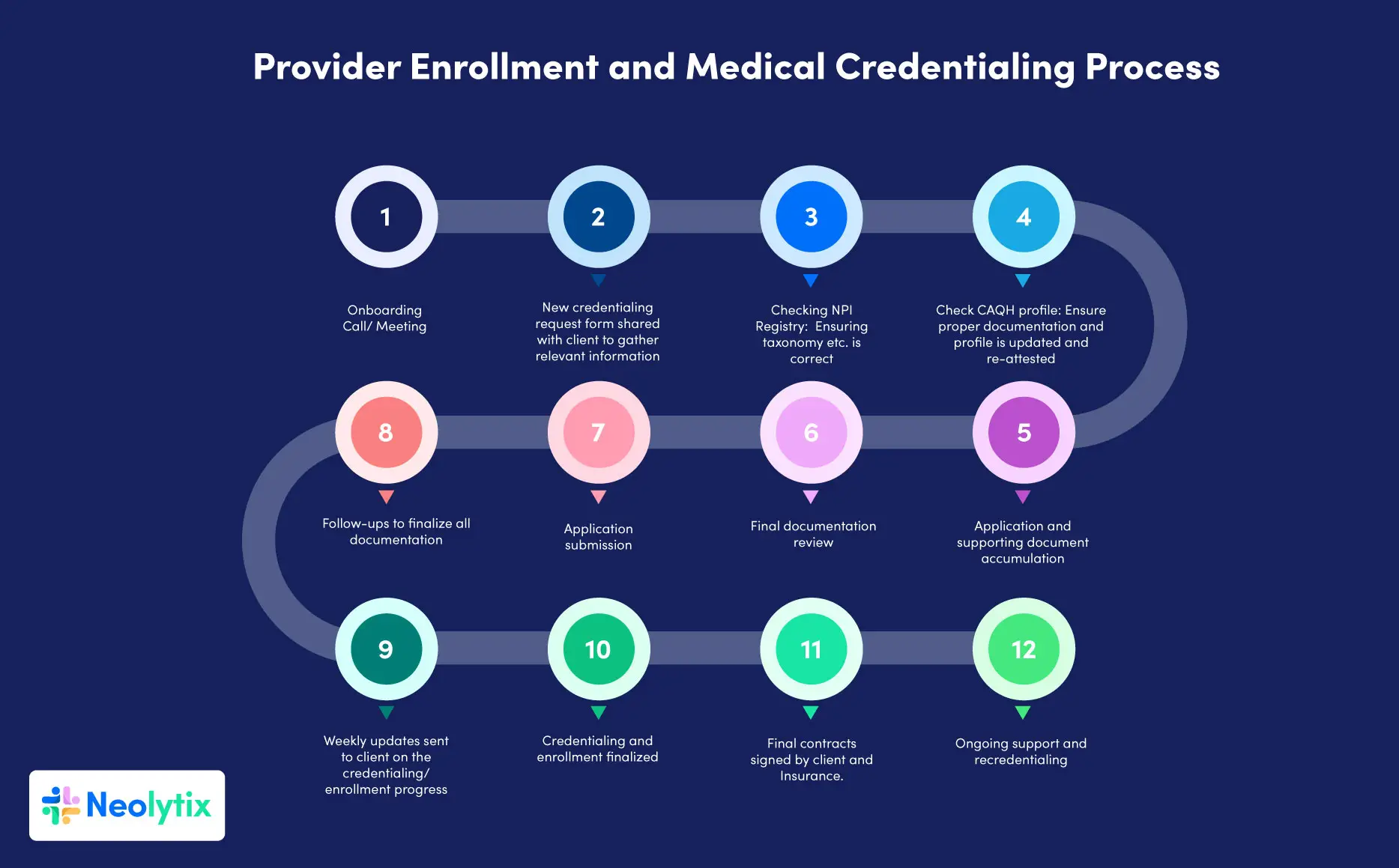
The Step-by-Step Credentialing Process
A defined step-by-step credentialing process is essential to ensure healthcare providers meet all necessary qualifications and standards. Here is an overview of the key steps involved:
Initial Application Review
Collect and review the initial application to ensure all required information is included. This includes personal details, educational background, training, work history, and references.
Primary Source Verification (PSV)
Verify credentials directly with the issuing institutions, such as medical schools, residency programs, and licensing boards. This step confirms the authenticity of the applicant’s qualifications.
Secondary Review
Conduct a thorough secondary review to identify any discrepancies or missing information from the initial application. This may involve cross-referencing details and following up on any inconsistencies.
Committee Review
Present the application and verification results to a credentialing committee for final approval. The committee typically includes experienced healthcare professionals who assess the applicant’s qualifications, experience, and competency.
Ongoing Monitoring
Continuously monitor the provider’s credentials to ensure they remain current. This involves tracking license renewals, board certifications, and any disciplinary actions or malpractice claims.
Credentialing for Physicians and Other Providers
The physician credentialing process requires a comprehensive review of education, training, licensure, and board certifications. A physician credentialing checklist ensures all steps are followed. Similarly, credentialing for medical providers maintains high standards of care.
Integration and Compliance
Integrating the medical provider credentialing process with other systems, like medical billing, ensures compliance and efficiency. The credentialing process for doctors must align with billing practices to prevent reimbursement issues.
Summary
Outsourcing the medical credentialing process for providers process offers numerous advantages to healthcare organizations. It allows facilities to focus on patient care while ensuring the accuracy and efficiency of the credentialing process. By partnering with experts like Neolytix, organizations gain access to specialized knowledge and advanced technology, which streamline credentialing procedures.
With 12 years of experience in helping healthcare practices across the country with enrollment and credentialing challenges, Neolytix is a trusted partner. Our expertise in the provider credentialing process ensures that your practice can reach its full potential.
Contact us today to explore how we can optimize your provider credentialing process flow and improve your organization’s efficiency.






