Healthcare Credentialing Services
Your Trusted Partner in Healthcare Credentialing Services
At Neolytix, we simplify and accelerate the complex process of provider enrollment and credentialing, helping healthcare organizations, group practices, and individual providers focus on patient care—not paperwork.
Every day your providers remain uncredentialed and unenrolled costs your organization approximately $9,000 in lost revenue. Our proven systematic approach has successfully processed over 8,000 providers with a 99.2% approval rate, transforming months-long processes into streamlined operations that get your providers practicing and billing faster.



Trusted by 270+ healthcare organizations nationwide






















Credentialing Verification Organization (CVO) Services
Credentialing Verification
also known as CVO Services—is the first and most critical step in the provider onboarding process. It involves verifying a healthcare provider’s qualifications to ensure they meet payer and regulatory requirements.
This comprehensive process includes:

Primary Source Verification:
Direct validation of education, training, licensure, board certification, work history, and malpractice history with original sources.

Compliance Alignment:
Ensuring adherence to NCQA and Joint Commission standards for quality and safety.

Ongoing Monitoring:
Continuous surveillance for sanctions, exclusions, and license expirations to maintain network eligibility.


Neolytix delivers enterprise-grade CVO services through our secure and automated inCredibly™ platform—ideal for healthcare systems, hospitals, IPAs, and multi-state medical groups.
Neolytix CVO Services Include:
- Automated primary-source verifications
- Real-time credentialing status updates
- Secure document collection and storage
- Sanction monitoring & expiration alerts
- Recredentialing and ongoing file maintenance
What Are the Steps Involved in Credentialing Verification?
Step 1:
Application Review
Foundation Analysis (Days 1-5)
- Identify missing documents and flag exceptions early
- Complete documentation gap analysis using comprehensive checklists
- Payer-specific requirement mapping for targeted accuracy
Step 2:
Primary Source Verification
Credential Authentication (Days 6-20)
- Confirm credentials directly with medical boards, licensing agencies, educational institutions, and certification bodies
- Expedited verification through established institutional relationships
- Digital verification tracking with real-time status updates
Step 3:
Centralized Document Retrieval
Information Recovery (Days 21-30)
- Through outbound calls and data requests, we complete any gaps in documentation
- Dedicated outbound team retrieving missing documents instantly
- Live database updates preventing information drift
Step 4:
Ongoing Monitoring & Re-credentialing
Continuous Compliance (Ongoing)
- Ensure continued compliance through routine re-verification and alert systems
- Automated deadline tracking preventing last-minute chaos
- Revalidation preparation starting 180 days in advance
Step 5:
Data Recording & Structuring
Information Management (Days 31-40)
- Maintain standardized and audit-ready records in payer and organizational databases
- Complete database synchronization with provider profiles
- Cross-platform data validation ensuring consistency
Step 6:
CAQH & Profile Maintenance
Sustained Accuracy (Ongoing)
- Keep provider information accurate and up to date according to payer and CAQH standards
- Quarterly attestations and license renewal tracking
- Continuous compliance monitoring against changing requirements
Our Latest Success Stories
Discover how Neolytix has driven remarkable revenue growth for healthcare providers through expert contract negotiation. Our most recent successes showcase the impact of our services, demonstrating substantial gains in CPT codes billed across a range of healthcare practices.
Top 3 billed codes
increase in reimbursement rate
• FirstCare | Texas
All billed codes
increase across all billed codes
• Caresource | Georgia
Top 5 billed codes
increase in CPT code billing
• BCBS | Texas
What Makes Neolytix the Right Choice
Neolytix has a top revenue management program to help you get the most value from the care you offer. Our team is comprised of seasoned professionals with in-depth knowledge of negotiating payer contracts.
14+ Years Experience
For more than 14+ years, Neolytix has helped healthcare providers nationwide fight for and win — fair reimbursement rates
100% Tailored Approach
Every practice is unique. We align our negotiation approach with your specialty, patient population, and financial goals for maximum impact
Nationwide Reach
Whether you’re a single-site practice or a multi-state organization, Neolytix has successfully negotiated contracts in all 50 states
10+ Insurers
UnitedHealth Group, Anthem, Aetna, Cigna, Humana, etc. We have negotiated with all the major players in the US.
Flexible Fee options
Choose between a fixed fee model for cost predictability or an incentive-based model where our success is tied to your results.
Case Studies
Real challenges. Measurable outcomes. or Proven Results Across Healthcare Operations
How a Practice Merger Led to a 20% Revenue Drop — and How We Recovered It
When a merged OB/GYN practice saw collections drop 20% post-merger, Neolytix uncovered four hidden operational failures: credentialing gaps, incomplete data migration, weak benefits verification, and poor denial oversight. A systematic intervention restored revenue to pre-merger levels — and beyond.
🏆 100% provider credentialing coverage | Revenue decline fully reversed within months | 95%+ benefits verification compliance
From Credentialed to Cash Flow - Provider Enrollment Excellence
Provider Enrollment is where credentialing meets revenue generation. We assist healthcare providers in enrolling with insurance networks, Medicare, Medicaid, and other payer organizations by completing and submitting enrollment applications with precision and speed.
Provider Enrollment Services Include:
Government Programs:
- Medicare & Medicaid Enrollment with expedited processing
- PECOS enrollment and ongoing maintenance
- State-specific program enrollment


Commercial Payer Networks:
- Major payer applications (BCBS, Aetna, UHC, Cigna, Humana)
- Regional and specialty payer enrollment
- Direct contract negotiations when applicable


Essential Registrations:
- NPI Registration & Management (Type I & II)
- CAQH Profile Setup & Maintenance
- ERA/EFT enrollment for seamless payments


Ongoing Management:
- Revalidations & Re-Credentialing coordination
- Facility and Group Enrollment Management
- Continuous payer communication and updates


Choose Full-Service RCM or Select Targeted Solutions — On Your Terms
Don’t have the appetite to harvest all the benefits from full-spectrum revenue cycle management solutions? No problem.
Select individual service offerings from within the revenue cycle to gain access to specific expertise to complement your non-clinical growth goals.
Incredible Credentialing. Revenue That Doesn't Wait.
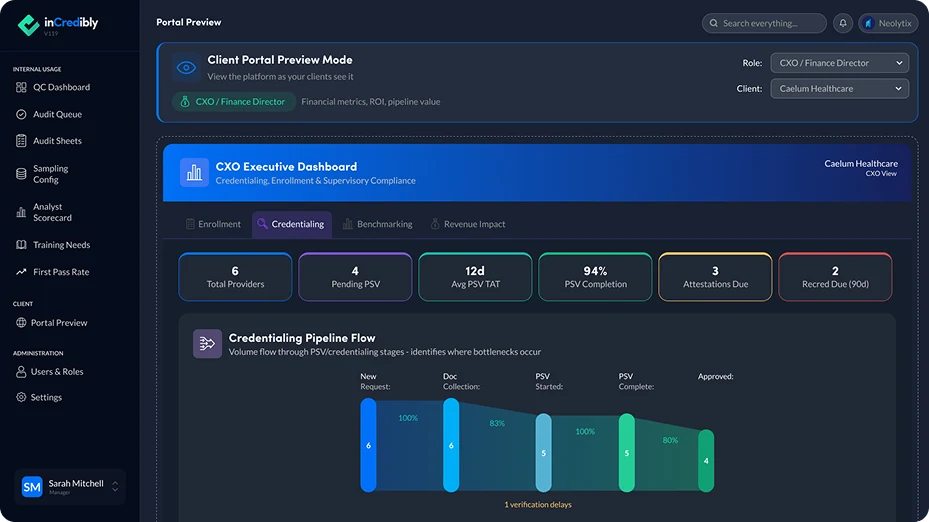
inCredibly™ is Neolytix’s purpose-built provider data intelligence platform, built to turn provider enrollment from an administrative holding pattern into a forecastable revenue pipeline.
Most enrollment tools tell you where an application is. inCredibly tells you when the provider will start billing and exactly how much revenue is at stake while you wait.
What inCredibly brings to your organization:
- Sankey Pipeline Visualization — identifies revenue-blocking bottlenecks across all active payer workflows
- Payer Intelligence Engine — verified submission contacts, current requirements, and process nuances updated daily
- Smart Data Extraction — pulls provider information from NPPES, state boards, and existing documentation automatically
- Time Allocation Analytics — shows where 40–60% of analyst effort is lost to avoidable follow-up
- Stakeholder Dashboards — COO, Recruiter, and MSO views with role-specific reporting

Still managing credentialing manually? Here's what it's costing you.
Our guide breaks down the hidden costs of manual credentialing, what automation actually changes, and the KPIs your team should be tracking today.
$45K–$150K
revenue lost per provider during a 90–120 day credentialing cycle
$45K–$150K
revenue lost per provider during a 90–120 day credentialing cycle
Why Choose Neolytix for Physician Credentialing Services?
Our credentialing services for hospitals, groups, IPAs, and healthcare organizations ensure that providers are fully compliant with industry standards, streamlining the process for both new and existing staff members.
Measurable Business Impact:

Revenue Recovery
Reduce revenue loss by getting providers credentialed faster. Save $27,000+ per provider through accelerated timelines and parallel processing of credentialing and enrollment.

Cost Reduction
Eliminate in-house credentialing costs averaging $20,000+ per provider annually in staff time and resources while improving quality and compliance.

Operational Efficiency
Free up 20+ hours per application of administrative time to focus on patient care and strategic growth initiatives.

Risk Mitigation
Reduce claim denials by 45% through accurate credentialing and comprehensive compliance management protocols.

Complete Transparency
Real-time tracking and reporting provide 100% visibility into credentialing progress with executive-level dashboards and predictive analytics.
The Economics of Credentialing Excellence
Your Current Reality:
- $9,000 daily revenue loss per uncredentialed provider
- $20,000+ annual internal credentialing costs per provider
- 180+ day average time-to-revenue for new providers
Your Neolytix Reality:
- 90-day average credentialing and enrollment completion
- 99.2% first-time approval rate
- Complete elimination of internal credentialing overhead
ROI Calculation: Most organizations see complete ROI within 60 days through accelerated revenue generation and eliminated internal costs.
Your Success is Our Success
Real testimonials from healthcare leaders who’ve partnered with us. See how we go beyond the expected to deliver results that make a difference.
I spoke with several billing companies, did my research, and Neolytix displayed the most compassion and flexibility of all of the companies we spoke with. We’ve worked together now for two years, and our practice has gone from two to six therapists; Neolytix has helped get us there. They’ve always been open to feedback and have been there to help make our processes run even smoother when we’ve run into bumps along the road. We are grateful for the whole team at Neolytix and know that they really care deeply about their clients.

Dr. Jenny Martin
Founder - Gemstone Wellness
The reason I chose Neolytix over other providers was how they handled the whole service process for me. I was particularly looking for expertise. I wanted to see reviews. I wanted to know that there were other clients that used this service and had an exceptional or outstanding experience… and you saw that with Neolytix.

Dr. Cresencia Felty
Founder - Natural Advancement Consulting
Neolytix is the most professional and hard working billing company I have ever been partners with . I call them a partner because they truly are. Neolytix makes sure what they bill is accurate. Their knowledge of physician billing is outstanding. The entire team takes control and does what is necessary to make sure you get paid.

Cheryl Lambert
Regional VP Finance - Prime Healthcare
We transitioned to Neolytix a while back, having come from a billing company we were less than thrilled about. The people here have been very responsive to our needs and requests, and adapt quickly to whatever curve balls our practice throws them. They bring a wealth of knowledge to the table, and take the attitude that our success is their success.

Toby Collins
Executive Director – Therapy Unlocked
I chose Neolytix for credentialing our practice. The team was knowledgeable, responsive and kind and supported us through the process. I would certainly recommend their services.

Sarah Charmchi
Founder/CEO – Serenity Psychotherapy Group
Neolytix has helped so much with our outstanding A/R. They are always so very willing to help and complete the task in a timely manner.

Sue Robbins
Rtd. Office admin – Riverview Pediatrics
We’ve been working with the Neolytix team since 2019, and I truly cannot recommend them enough. This is not a massive company that treats you like just another account — this is a tight-knit, professional, and compassionate team that works closely with you, hand in hand. The team is always available, quick to respond, and consistently goes above and beyond to make sure we’re supported.

Yasser Rivera
General Manager – BG Medical Center
Our practice has been a customer for almost 2 years. I highly recommend this company, especially for new startup medical practices like ours. We were advised on steps to take from day 1, and Ritu walked us through all the steps…all the way. The billing team is fantastic, we are happy with the services.

Abosede Woody
NP, Mathers Clinic LLC
Security-First. At Every Step.
Built for Compliance. Designed for Confidence.
Every service we deliver is built on a foundation of strict data governance and regulatory compliance. HIPAA safeguards and ISO 27001-certified security practices are embedded into how we work, not added after the fact.


Get in touch with us
The Questions Healthcare Leaders Ask ( FAQs)
How do you handle both credentialing AND enrollment simultaneously?
Our integrated approach treats credentialing and enrollment as complementary processes, not sequential ones. We submit enrollment applications as soon as primary source verification is complete, cutting total time-to-revenue by 45-60 days.
What if we have providers stuck in credentialing limbo right now?
We specialize in credentialing rescue operations. Our team will assess stuck applications, identify roadblocks, and implement recovery protocols. Most “impossible” cases just need expert intervention and direct payer relationships.
Can your platform integrate with our existing systems?
inCredibly™ is built for integration. We connect with major practice management systems, EHRs, and credentialing databases. Our technical team handles all integration work—no IT burden on your side.
What about ongoing maintenance and revalidation?
That’s where we truly shine. Our platform automatically tracks all renewal dates, sends advance warnings, and manages the entire revalidation process. You’ll never miss a deadline or face a compliance lapse again.
Ready to Accelerate Your Credentialing?
Stop losing $9,000 per day per uncredentialed provider. Let Neolytix take the complexity off your plate—so your team can focus on growth and patient care.
Here’s what happens next:
- Free Credentialing Assessment – Complete analysis of your current processes with improvement recommendations
- Custom Implementation Plan – Detailed roadmap showing timeline and ROI projections
- Platform Demo – Live demonstration of inCredibly™ and how it transforms your workflow
Ready to transform provider credentialing from your biggest operational headache into your competitive advantage? Your providers want to practice medicine, not navigate bureaucracy. Your CFO wants predictable revenue, not credentialing excuses. You want a partner who delivers results.
That’s exactly what we do.





