Medical Credentialing.
Faster Revenue
InCredibly replaces the guesswork in credentialing, enrollment, and licensing with date-certain timelines that leadership can plan around. Neolytix manages the entire process end-to-end and through InCredibly, executives see exactly when each provider will be credentialed, enrolled, and ready to bill.
Instead of chasing status updates and managing around uncertainty, leadership operates with specific dates that drive confident hiring decisions, accurate revenue forecasts, and faster time-to-revenue.
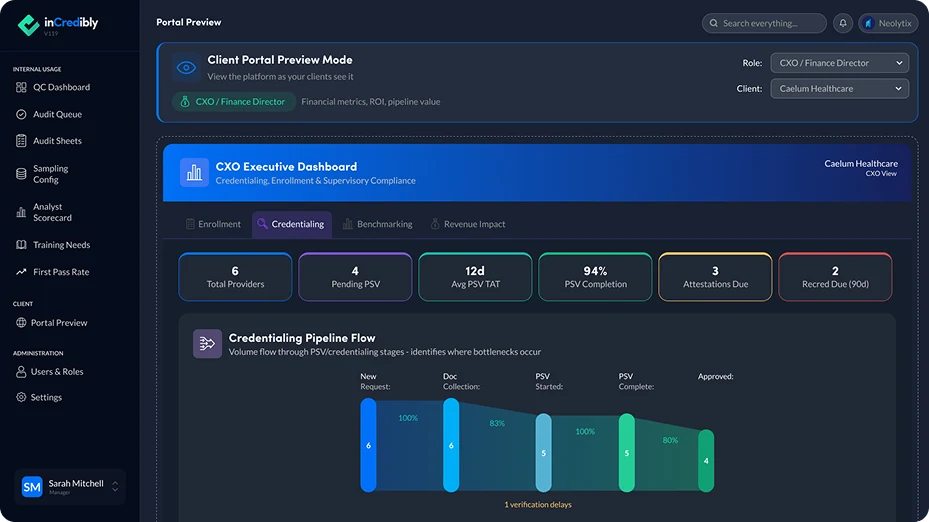
Credentialing Undermines Revenue Forecasting
Credentialing and enrollment failures don’t simply slow provider onboarding — they remove visibility from the systems leaders rely on to plan revenue, staffing, and growth. When timelines are unclear, organizations lose the ability to forecast accurately, manage risk proactively, or explain revenue variance with confidence.
What appears operational on the surface becomes a financial and strategic blind spot at scale.
Unpredictable Credentialing Timelines
Providers typically wait 90–120+ days to become billable, with some exceeding 180 days, making go-live planning unreliable across payers and states.
Providers Hired but Unable to Bill
33% of organizations report credentialing delays of 30–45 days, and 18% face delays beyond 60 days, leaving providers paid but non-billable.
Revenue Lost to Administrative Lag
Credentialing and enrollment delays can cost up to $122,144 per physician, while facilities lose approximately $10,122 per provider per day during enrollment bottlenecks.
Limited Leadership Visibility
With 52% of workflows still manual, credentialing status is spread across emails, spreadsheets, and portals—limiting readiness insight and early intervention.
When credentialing timelines are unclear, operations lose control and finance absorbs the cost.
A Modern Provider Data Intelligence Platform for Scalable Credentialing Outcomes
Timeline Certainty for Operational Leaders
Credentialing fails when leaders can’t answer one simple question: When will this provider be ready to work and bill?
InCredibly replaces status ambiguity with structured, forecastable timelines – organized by payer and provider patterns – so readiness becomes predictable, not reactive.
What this enables:
- Timeline forecasting by payer and provider
- Early alerts when timelines begin to slip
- Go-live dates leadership can plan around
Reduce Credentialing Drag on Revenue
Every day a provider cannot bill is lost revenue. Credentialing delays don’t just slow operations – they slow cash flow.
InCredibly connects credentialing progress directly to financial impact, making revenue timing visible and measurable.
Revenue-Focused Outcomes
- Faster provider billing readiness
- Fewer idle provider days
- Reduced retroactive billing risk
- Clear visibility into revenue readiness
Reduce Revenue Drag
Cardiology
Neurology
Traditional
InCredibly
Traditional
InCredibly
What Is InCredibly?
InCredibly is a centralized orchestration and intelligence platform for credentialing, enrollment, and licensing, built on top of Neolytix’s fully managed end-to-end services.. It is designed to deliver predictable timelines, scalable execution, and leadership‑level visibility.
Organizations gain not just operational support, but real-time insight into provider readiness, bottlenecks, and revenue impact across the full onboarding lifecycle.
Not just credentialing execution — credentialing control .

Reduction in credentialing turnaround

Reduction in manual effort

Years healthcare credentialing expertise
Coordinated Credentialing and Enrollment Workflows
InCredibly unifies credentialing and payer enrollment workflows into a single system so healthcare leaders can see readiness, risk, and revenue impact in one place.

Credentialing
Manage provider credentialing and privileging with structured workflows, real-time status tracking, and leadership-level visibility – so teams know where providers stand and when they are expected to be ready.

Enrollment
Support payer enrollment with accurate submissions and clearer visibility into billing readiness, helping organizations understand when providers can begin generating revenue.
Capabilities That Preserve Performance at Scale
Built for Multi-Entity Healthcare Organizations
InCredibly is designed for organizations managing credentialing across multiple providers, locations, and stakeholders, with visibility tailored by role.
Operations
Track progress, timelines, and escalations across payers and providers.
Finance
See when providers become billable and where revenue is delayed.
Leadership
Understand system-level readiness, risk, and revenue exposure.

Together, these workflows provide a consolidated view of provider onboarding — from initial credentialing through operational readiness.
Always Audit-Ready. Never Scrambling.
Compliance is incorporated directly into credentialing and enrollment workflows rather than treated as a separate or downstream activity. Required documentation, verification steps, and approvals are tracked as part of day-to-day work.
Trusted by 270+ organizations across the globe
Overall Satisfaction
“We are grateful for the whole team at Neolytix and know that they really care deeply about their clients.”
Selection Process & Differentiation
“From the beginning there was a group meeting, I got to meet everyone on the team. I was immediately supported but not overwhelmed with the process. They were very clear and organized, and that is what made me want to continue working with Neolytix.“
“Neolytix is the most professional and hard working billing company I have ever been partners with . I call them a partner because they truly are. Neolytix makes sure what they bill is accurate. Their knowledge of physician billing is outstanding. The entire team takes control and does what is necessary to make sure you get paid.”
“We transitioned to Neolytix a while back, having come from a billing company we were less than thrilled about. The people here have been very responsive to our needs and requests, and adapt quickly to whatever curve balls our practice throws them. They bring a wealth of knowledge to the table, and take the attitude that our success is their success.”
— Sandy
“We’ve been working with the Neolytix team since 2019, and I truly cannot recommend them enough. This is not a massive company that treats you like just another account — this is a tight-knit, professional, and compassionate team that works closely with you, hand in hand. The team is always available, quick to respond, and consistently goes above and beyond to make sure we’re supported.”
“Our practice has been a customer for almost 2 years. I highly recommend this company, especially for new startup medical practices like ours. We were advised on steps to take from day 1, and Ritu walked us through all the steps…all the way. The billing team is fantastic, we are happy with the services.”
Frequently Asked Questions
Many organizations outsource execution to reduce administrative burden, access specialized expertise, and maintain consistency across payers and states. Platforms like InCredibly are designed to support and systematize these workflows by providing structure, visibility, and retained institutional knowledge.
Credentialing timelines vary based on payer requirements, provider specialty, completeness of data, and state regulations. Industry benchmarks commonly range from several weeks to multiple months, which is why predictability and visibility are critical.
InCredibly supports CAQH‑related workflows by centralizing data, tracking requirements, and improving visibility into readiness. Specific submission and maintenance responsibilities depend on organizational processes.
Hospitals often outsource to manage scale, reduce operational strain, improve compliance consistency, and mitigate the impact of staffing turnover while maintaining oversight and control.
Accurate credentialing and timely enrollment help reduce downstream issues such as delayed billing and eligibility‑related denials by ensuring providers are properly credentialed before services are rendered.
Implementation timelines vary based on organizational complexity, payer mix, and the scope of workflows being configured. For most organizations, initial implementation is completed within approximately 2–5 days, with timing adjusted based on structure, volume, and onboarding requirements.
Revenue impact typically begins to emerge as onboarding delays are reduced, and billing readiness becomes visible earlier in the credentialing and enrollment process.
Most organizations start to observe measurable improvements within approximately 3–6 months, depending on factors such as provider volume, payer mix, and existing operational maturity. The timing and magnitude of impact vary by organization and implementation context.
InCredibly is designed for multi‑entity, multi‑state healthcare organizations.
Through centralized documentation, structured workflows, and visibility designed for audit readiness.
Leadership gets a transparent view of what is happening across the organization, combining an eagle’s-eye view of credentialing and enrollment progress with the ability to access in-depth analytics when deeper review is needed. This visibility spans functions involved in provider onboarding, helping leaders understand readiness, timelines, and constraints without relying on isolated task-level updates.