Understanding Charge Entry in Medical Billing
The vital role of charge entry in medical billing is often underestimated, but it presents opportunities to contribute to improved revenue and efficiency within the revenue cycle. In this guide, we will unravel the essence of charge entry—what it entails, where it stands in the billing process, the critical significance of accuracy, and its far-reaching impact on payors, patients, and healthcare providers.
Additionally, we will delve into the nitty-gritty of the charge entry process, offering practical insights to enhance accuracy.
What is Charge Entry?
Charge entry in medical billing represents the meticulous translation of healthcare services into coded entries for billing purposes. It goes beyond mere data entry; it is a meticulous process where each service, from routine check-ups to intricate surgeries, is carefully recorded to ensure that billing accurately mirrors the care provided.
Where Charge Entry Fits into the Billing Process
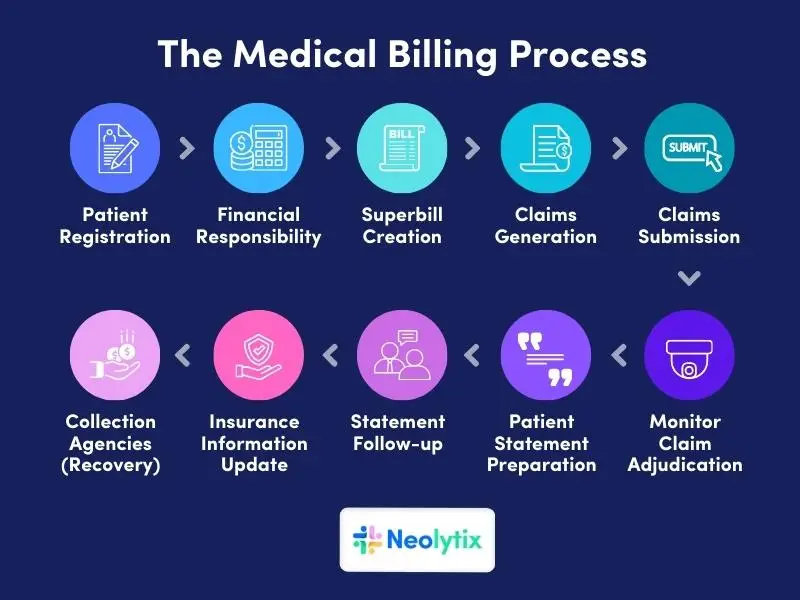
The medical billing process consists of 10 steps and the charge entry process can span over multiple steps, depending on the individual organization’s billing process, and creates a comprehensive record of billable items, serving as the foundation for subsequent claim generation and submission.
In short, charge entry follows the gathering of patient demographics, the assignment of medical codes, the submission of claims and subsequent monitoring and mitigation thereof. It’s similar to assembling the pieces of a financial puzzle, ensuring that every service is accounted for and billed correctly.
The Importance of Accurate Charge Entry
- Optimizing Revenue
Accurate charge entry is the bedrock for revenue optimization in medical billing. It guarantees that healthcare providers receive fair reimbursement, contributing to the financial health of the organization. It’s not just about getting paid; it’s about getting paid the right amount for the services rendered.
- Minimizing Claim Denials
Error-free charge entry acts as a shield against claim denials. Precise billing records significantly reduce the risk of denials, avoiding reimbursement delays and administrative complications. A denied claim not only delays revenue but can also strain provider-payer relationships. Accurate charge entry helps maintain the fluidity of this crucial financial transaction.
- Enhancing Patient Satisfaction
Transparent and accurate billing resulting from precise charge entry contributes to patient satisfaction. In an era where patients are becoming more financially aware and engaged, clear and accurate billing provides them with a sense of transparency and control over their healthcare expenses.
- Supporting Payor Relations
Trust is paramount in payor-provider relationships. Accurate charge entry builds trust by aligning billed charges with the services rendered, creating a foundation for efficient financial transactions. It’s not just about a financial transaction; it’s about building a relationship based on mutual trust and understanding.
The Charge Entry Process in Detail
1. Patient Demographics
Accurate patient information is the starting point for charge entry. Thorough and up-to-date records ensure that the subsequent charge entry aligns with the actual services provided, reducing errors in billing. Patient demographics go beyond mere names and addresses; they include insurance information, ensuring that the right payor is billed for the services rendered.
2. Coding Teams
Trained coding teams play a pivotal role in charge entry. They interpret medical services into standardized codes, bridging the gap between provided services and accurate billing. Continuous training ensures their skills remain current, aligning with evolving coding guidelines. Coding is not a static task; it’s a dynamic process that requires constant learning and adaptation to ensure accuracy in charge entry.
3. Charge Entry Process
This step involves inputting coded information into the billing system, creating a detailed record of billable services. Precision at this stage is crucial, as it forms the basis for downstream billing processes. It’s not just about data entry; it’s about translating complex medical procedures into a language that billing systems and payors can understand.
4. Medical Codes
Accurate coding is the backbone of charge entry. Properly assigned codes ensure that billed services are reflective of the actual care provided, reducing the risk of underbilling or overbilling. Regular training and updates for coding teams are essential to maintaining accuracy in this critical aspect.
Coding training and coding audits complement each other. It is the best way to test the proficiency of your coding operations to detect any opportunities where coding training is required.
How to Improve Charge Entries
- Regular Training for Coding Teams: Ongoing training keeps coding teams well-versed in changing coding guidelines, enhancing accuracy in code selection during the charge entry process. This investment in human resources is crucial for maintaining a high standard of accuracy. Training is not just a one-time event; it’s a continuous process that acknowledges the dynamic nature of medical billing and coding.
- Thorough Audits of Charge Entry Records: Regular audits are essential for identifying and rectifying errors in charge entry records. A proactive approach to auditing maintains a high level of accuracy, minimizing revenue leakage and avoiding potential claim denials. Audits are not just about finding mistakes; they are about creating a culture of accountability and continuous improvement in charge entry processes.
- Implement Cross-Functional Collaboration Workshops: Encourage collaborative workshops that bring together coding teams, billing specialists, and healthcare providers. These sessions facilitate open communication and understanding of each team’s role in the charge entry process. By promoting cross-functional collaboration, organizations can address potential challenges at the intersection of coding and billing.
- Utilize Advanced Billing Software: Implementing cutting-edge billing software streamlines the charge entry process. Automation reduces manual errors, enhances efficiency, and ensures a smoother workflow. It’s not just about adopting technology; it’s about leveraging it to enhance accuracy and streamline operations, ensuring that charge entry becomes a seamless part of the broader billing process.
- Automate Error Detection: Leverage technology detects errors in charge entry automatically. Automated error detection allows for immediate correction, reducing the likelihood of claim denials and streamlining the overall billing process. If the system identifies any discrepancies or errors during the validation process, it flags them for review. Common errors may include incorrect medical codes, missing patient information, or discrepancies in service details. Automation is not just about saving time; it’s about enhancing accuracy by minimizing the impact of human error in charge entry.
Conclusion
By embracing precision in charge entry, healthcare providers can unlock financial stability, build trust with payors, and enhance patient experience. It is a vital part of the medical billing process that is often neglected but impacts a healthcare organization’s revenue potential and cash flow.
Neolytix has been at the forefront of helping healthcare organizations optimize their medical billing and coding processes for over 12 years. Schedule a free demo and learn how our medical billing solutions can provide tailored solutions to your healthcare organization and to cement its future financial prosperity.
Author
-
Rajat Bhatnagar is a healthcare technology innovator and CEO of Neolytix. With expertise in digital health, revenue transformation, and practice management, he has led initiatives that drive efficiency, automation, and growth for healthcare providers nationwide. Passionate about integrating business strategy with technology, Rajat continues to shape solutions that empower practices to deliver better care while thriving in an evolving healthcare landscape.






