Ophthalmology Medical Billing & Coding Guide (2026)
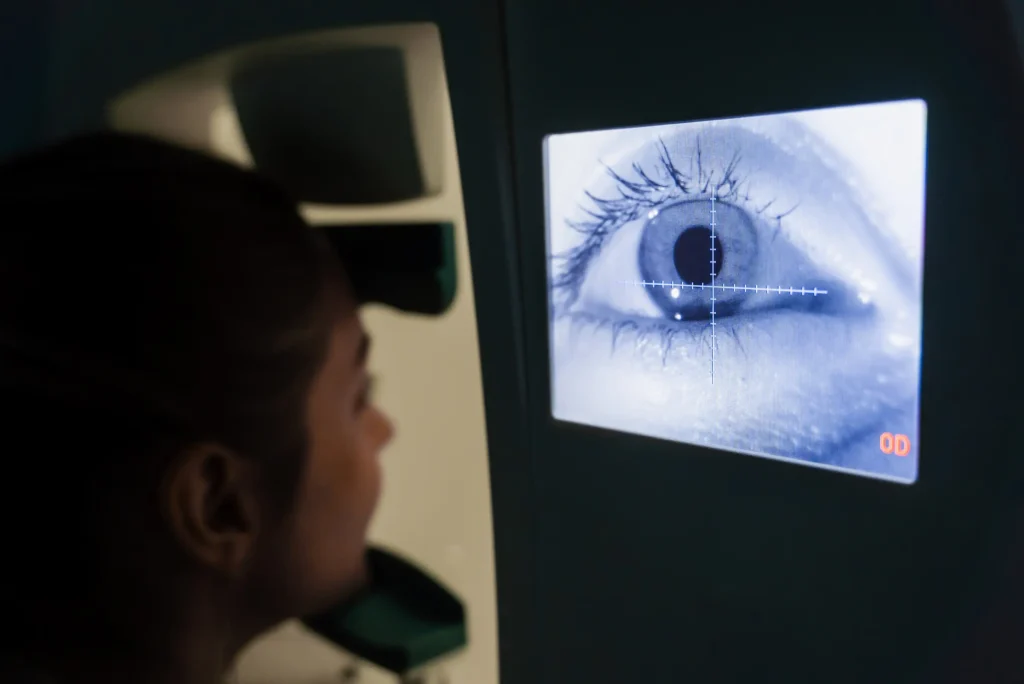
Simplify Processes, Maximize Reimbursements, Empower Care Ophthalmology is a specialized branch of medicine focused on the diagnosis, treatment, and management of disorders related to the eyes and visual system. Ophthalmologists provide both medical and surgical care for conditions affecting the eye, eyelids, tear ducts, and surrounding structures. Ophthalmology medical billing and coding require the accurate […]
Denial Codes in Medical Billing: Complete List and What They Mean

Every denied claim costs your practice more than the reimbursement it represents. According to a 2025 MDaudit report, the average amount tied to a single medical necessity denial has climbed to $450, a 70% increase over the prior year, while average denied inpatient claims rose 12% from 2024 to 2025. For practices already working with thin margins, that […]
What Is a Clean Claim in Medical Billing? (And Why It Matters)

Healthcare providers submit billions of claims every year. Yet according to Experian Health’s State of Claims 2025 report, the initial claim denial rate hit 11.8% in 2024, up from 10.2% just a few years prior. More telling: industry analysis estimates that reworking a single denied claim now costs providers anywhere from $25 to $181 in administrative labor. Over time, that math becomes unsustainable for any practice operating on […]
Orthopedics & Musculoskeletal Medical Billing & Coding Guide (2026)
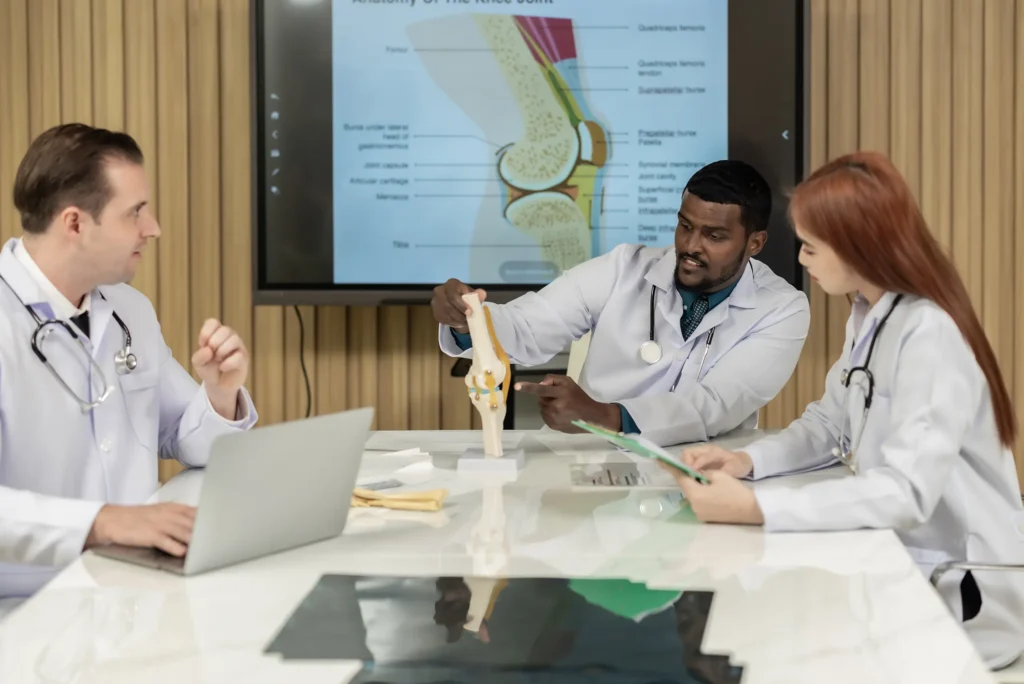
Simplify Processes, Maximize Reimbursements, Empower Care Orthopedics is a medical specialty focused on the diagnosis, treatment, and management of conditions affecting the musculoskeletal system — including bones, joints, muscles, ligaments, tendons, and connective tissues. Orthopedic physicians treat a wide range of conditions such as fractures, arthritis, joint injuries, spine disorders, sports injuries, and degenerative musculoskeletal […]
The Complete Guide to Denial Management in Medical Billing

Every denied claim represents revenue a healthcare organization has already earned but not yet received. For many practices, that gap is larger than they realize. Initial claim denial rates reached 11.8% in 2024, up from 10.2% in 2020, and U.S. hospitals alone lose an estimated $262 billion annually to initial claim denials. What makes this figure particularly striking is […]
What Is Medical Billing? A Guide for Healthcare Providers

Medical billing is the financial backbone of every healthcare practice in the United States. Yet for many providers, it remains one of the least understood functions in their organization, until it breaks down. Claim denials climb, reimbursements stall, and revenue starts to erode, often without a clear explanation of where the process went wrong. The scale of […]
The Ultimate Guide to Credentialing Technology

Overview Provider credentialing sits at the intersection of revenue, compliance, and patient safety — yet most healthcare organizations still manage it manually. The result: 90–120 day cycle times, $45,000–$150,000 in revenue loss per provider, and growing exposure under NCQA’s 2025 standards, which now mandate monthly sanctions monitoring and shortened verification windows. This guide examines the […]
Credentialing for Health Systems: Managing High-Volume Provider Onboarding

Health systems are hiring at scale. Physician shortages, service line expansions, post-merger integrations, and telehealth growth are driving provider rosters into the hundreds — sometimes thousands — across multiple facilities and states. But the credentialing infrastructure supporting that growth was rarely built for it. According to a 2025 industry survey of over 500 provider-based healthcare organizations, […]
What Is NPPES? A Guide to NPI Numbers, Registration & Verification

When CMS compared provider information in payer machine-readable files against the NPPES NPI registry, only 28% of provider names, addresses, and specialties matched. That gap is not a data quality footnote — it is the operational reality behind delayed enrollments, rejected claims, and providers who are credentialed but unable to bill. At the center of […]
Group Practice Credentialing Explained: A Practical Guide for Medical Groups

Running a medical group means managing more than patient care. It means managing the operational infrastructure that keeps care billable, compliant, and scalable. At the center of that infrastructure is group practice credentialing, a process that is frequently underestimated in complexity and overestimated in simplicity. The stakes are not abstract. Industry research shows that credentialing and payer […]