Remote patient monitoring reimbursements are helping the technology grow beyond expectations. Recent studies revealed that the RPM market is set to grow at a CAGR of 16.47% until 2027, reaching USD 60.31 million by 2027.
COVID-19 incited the growth spurt of RPM, but now, another motivator beyond improving patient outcomes is driving the uptake of RPM. During unprecedented times of inflation, a labor shortage, and payors gripping their wallets even tighter, healthcare organizations are searching for ways to optimize their revenue cycles.
But now, RPM reimbursement provides a fresh breeze of revenue without draining the organization’s resources. Of course, patient outcomes, as well as the patient experience, improve as well, which makes RPM even more attractive.
What's the difference between Remote Patient Monitoring (RPM) and Remote Therapeutic Monitoring (RTM)?
Remote Patient Monitoring (RPM) and Remote Therapeutic Monitoring (RTM) are related concepts, but they focus on different aspects of healthcare. In summary, while both RPM and RTM involve remote monitoring, RPM is more comprehensive, monitoring overall health parameters, while RTM is specifically focused on tracking a patient’s response to a particular therapeutic intervention.
- Remote Patient Monitoring (RPM)
RPM involves the use of technology to monitor and collect medical and health-related data from patients in one location and transmit it to healthcare providers in another location. The primary goal of RPM is to track and manage patient’s health outside of conventional healthcare settings. It is often used for patients with chronic illnesses or those in post-acute care.
Examples: Monitoring vital signs (such as blood pressure, heart rate, and oxygen levels), glucose levels for diabetic patients, and other health metrics. RPM helps in early detection of health issues and allows for timely intervention.
Note: Sometimes insurers like Aetna and even CMS refer to RPM as ‘Remote Physiologic Monitoring.’
- Remote Therapeutic Monitoring (RTM)
RTM involves monitoring patients’ response to a specific therapeutic intervention or treatment remotely. It focuses on tracking the effectiveness and safety of a particular medical treatment. The goal of RTM is to ensure that a therapeutic intervention is producing the desired outcomes while minimizing negative effects. It involves continuous or periodic monitoring during the course of treatment.
Examples: Monitoring a patient’s response to medication, tracking side effects, assessing the impact of a medical procedure, or observing the progress of rehabilitation therapy. RTM is specific to the therapeutic aspects of patient care.
Remote Patient Monitoring (RPM) Reimbursement By Medicare
The amounts illustrated below is the Medicare national average and it should be noted that the amounts may change over time. But given these reimbursement amounts, it is easy to see how RPM reimbursements can provide a significant amount of extra reimbursement revenue.
According to CMS, for both RPM or RTM, only one practitioner can bill CPT codes 99453 and 99454, or CPT codes 98976, 98977, 98980, and 98981, during a 30-day period. Also, only when at least 16 days of data have been collected on at least one medical device. Also, RPM and RTM can’t be billed together.
For more information, read the Final Rule of 2024.
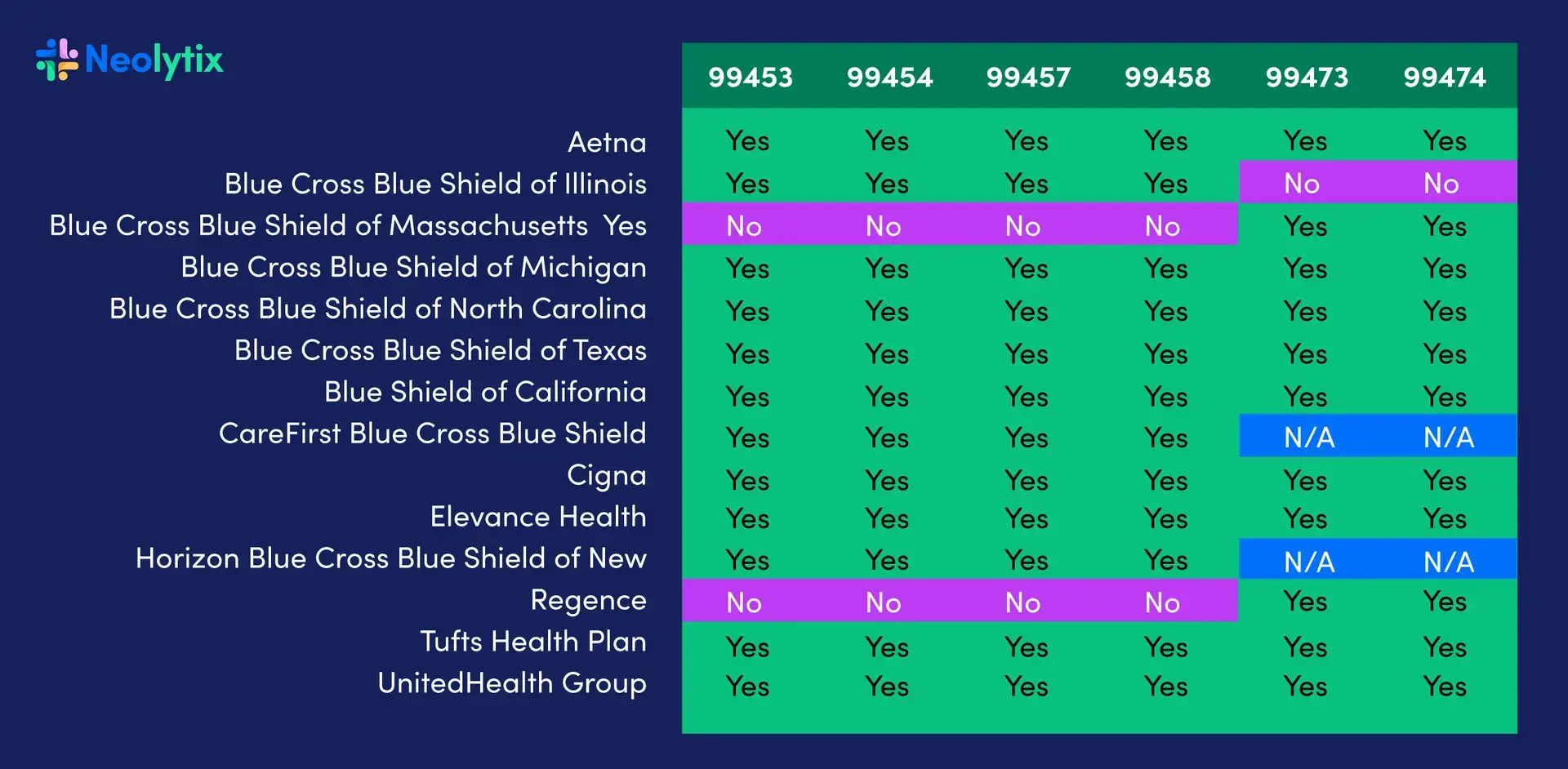
Remote Patient Monitoring (RPM) Reimbursements By Private Insurance Companies
As the table above shows, significant insurers like Cigna, UnitedHealth Group, Aetna, etc., offer reimbursements for all CTP code claims. In contrast, others like Regence offer reimbursement for remote patients for specific CPT codes only.
According to the American Medical Association, uneven acceptance of digital medicine CPT codes is observed in the commercial market. Some plans have clear clinical coverage policies, while others may not explicitly state coverage policies but might still reimburse claims for the codes when billed by healthcare professionals.
Health plans lacking explicit policies often default to state regulations, where specific coverage requirements may be outlined for state-regulated commercial plans. Most payers widely cover remote patient monitoring and are still considering coverage for newer remote therapeutic monitoring codes payers.
The Future Of Remote Patient Monitoring (RPM)
If we consider that 6 in 10 adults in the US have a chronic disease, and that 4 in 10 have two ore more chronic diseases, it is understandable why National Health Expenditure (NHE) grew by 4.1% in 2022 and accounted for 17.3% of Gross Domestic Product.
In the same period, Medicare spending grew 5.9% and Medicaid spending grew 9.6%.
Now let’s take the US’s aging population into consideration. The projected growth indicates that the population of individuals aged 65 and above in the United States is expected to rise from 58 million in 2022 to 82 million by the year 2050, reflecting a 47% increase.
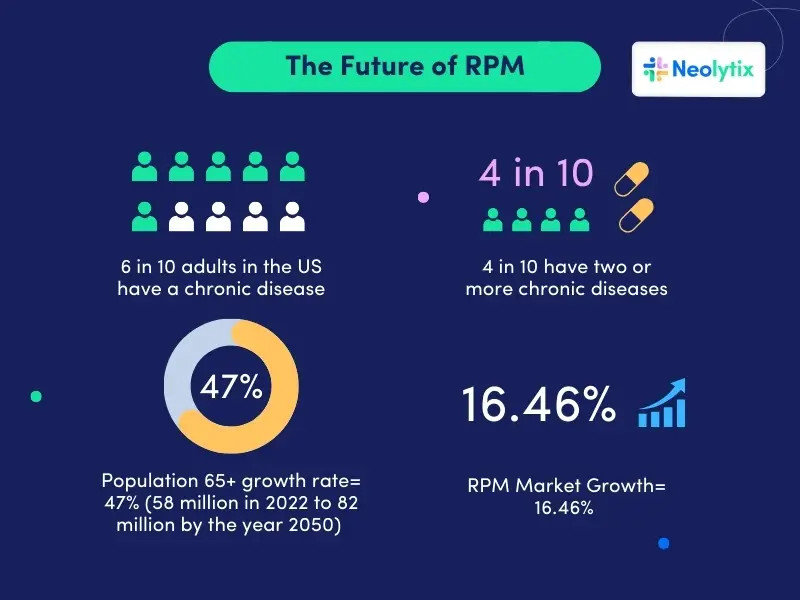
Given these statistics, it is clear why, as we stated at the beginning of the article, RPM will continue to grow at a CAGR of 16.47%. Healthcare organizations and practices can rest assured that RPM isn’t just a passing trend; it is here to stay and will continue to grow as an integral part of healthcare in the US.
If you want to learn more about the Remote Patient Monitoring (RPM) Program, schedule a free demo today.






