A small cardiology group in suburban Atlanta couldn’t understand why their revenue dropped $75,000 in Q1 2026. Same patient volume. Same procedures. Same Medicare mix.
Yet the numbers told a brutal story: they were earning less for the exact same work.
The culprit wasn’t poor performance—it was the fifth consecutive year of Medicare physician payment cuts, compounded by 270 new CPT codes, 38 revisions, and 112 deletions. This perfect storm of reimbursement challenges is affecting healthcare organizations nationwide.
For organizations already operating on razor-thin margins, the 2026 Medicare reimbursement squeeze isn’t just an administrative headache—it’s an existential threat that demands immediate, strategic action.

The Numbers Behind the 2026 Medicare Payment Crisis
Understanding the Conversion Factor Collapse
The Medicare Physician Fee Schedule conversion factor dropped from $33.29 in 2024 to $32.35 in 2026—a 2.83% decrease, marking the fifth straight year of reductions.
But the real impact is deeper:
- Adjusted for inflation, Medicare physician payment rates have fallen 29% since 2001.
- Practice expenses have increased 39% during the same period.
- CMS projects an additional 3.6% increase in practice costs for 2026, creating an effective cut of over 6%.
For example, a healthcare organization with $5 million in annual Medicare revenue faces:
- $141,500 in direct losses from the conversion factor cut
- Over $320,000 in total negative financial impact when factoring in rising costs
For many organizations with narrow margins, this is the difference between breaking even and operating at a loss.
The CPT Code Complexity Multiplier
How 420 Code Changes Amplify Revenue Loss
The 2026 CPT update includes:
- 270 new codes
- 38 revisions
- 112 deletions
Key changes include:
Telemedicine Overhaul
New codes (98008–98015) replaced old telephone evaluation codes (99441–99443). CMS initially signaled Medicare might not reimburse these codes, creating uncertainty for telehealth-heavy specialties.
Surgical Updates
New autologous skin cell suspension codes (15011–15018) support advanced wound care. New code 25448 simplifies carpometacarpal suspension arthroplasty reporting.
Diagnostic Changes
Three ophthalmic diagnostic tests received generous raises in 2026: fluorescein and ICG angiography (92242), ICG angiography (92240), and temporary amniotic membrane placement (65778).
Without updated coding workflows, organizations risk significant denials, delayed payments, and compliance issues
The Documentation Time Bomb
Proper documentation has never been more critical—or more complex. Medicare’s stricter medical necessity requirements, coupled with AI-driven claim reviews, leave almost no room for error.
Inadequate documentation can trigger denials or payment delays if carriers request additional information. Claims must not only support the procedures performed but also clearly demonstrate medical necessity with accurate diagnosis codes, clinical indicators, and treatment rationale.
The Denial Epidemic Crushing Healthcare Revenue
Denial Rates Hit Crisis Levels
Lower reimbursement isn’t the only problem—claim denials are compounding revenue losses.
- Initial claim denials hit 11.8% in 2025, up from 10.2% a few years earlier.
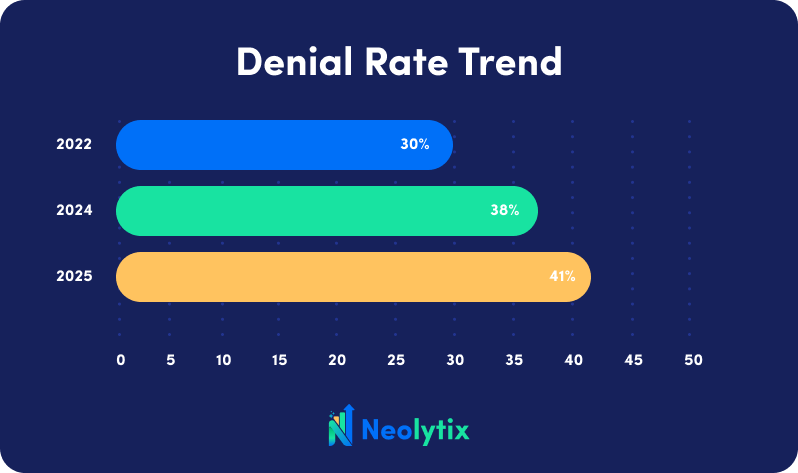
- By 2026, 41% of providers reported more than 10% of their claims denied, compared to 38% in 2025.
- Medicare Advantage initial denials averaged 15.7–17%.
Impact Example:
An organization submitting 10,000 Medicare claims per month at an average reimbursement of $250 per claim faces potential denials totaling $425,000 monthly. Even if 57% of denied claims are ultimately overturned, administrative appeal costs often exceed recovered revenue, resulting in a 7% net reduction in Medicare Advantage revenue.
Strategic Survival: How to Protect Your Revenue in 2026
1. Master CPT Code Changes Before They Cost You
- Update coding workflows for CPT/HCPCS/ICD-10
- Prioritize high-volume, high-risk codes
- Follow MACs’ Local Coverage Determinations (LCDs)
2. Build Front-End Accuracy Into Patient Access
- Real-time eligibility verification
- Automated demographic checks
- Insurance discovery tools
- Financial counseling
3. Deploy Pre-Submission Claims Scrubbing
- AI-enabled scrubbing can reduce denials by 30–40%, accelerating clean-claim rates and reimbursement timelines.
4. Optimize Denial Management
- Track denials by payer and reason
- Appeal high value claims only
- File appeals within 120 days
- Leverage AI to predict appeal success
5. Partner With Expert RCM Services
Many organizations now rely on professional RCM partners to:
- Reduce denials, improve cash flow, maintain coding accuracy
- Strengthen compliance and ensure continuous billing amid staffing shortages
Neolytix: Your Partner in Revenue Cycle Optimization
Neolytix provides the operational and financial infrastructure healthcare organizations need to stay profitable.
Services include:
- Full-Service Revenue Cycle Management: End-to-end billing, claims management, AR follow-up, payment posting, and reporting
- Certified Coding & Compliance: CPT/ICD-10 coding aligned with 2026 updates and payer rules
- Denial Prevention & Recovery: AI-backed scrubbing, automated tracking, root-cause analysis, optimized appeals
- Advanced Automation: Streamlined eligibility checks, prior authorizations, claim edits, AR workflows
- Analytics & Transparency: Real-time dashboards, KPI tracking, actionable insights
Neolytix functions like an outsourced COO, strengthening the operational backbone of healthcare organizations nationwide.
Looking Ahead: The 2026 Outlook and Beyond
The challenges don’t end in 2025. A temporary 2.5% physician payment increase is scheduled for 2026 but won’t retroactively offset 2025 cuts.
Without permanent Medicare reform, the cycle of cuts and temporary patches will continue. The AMA supports the Strengthening Medicare for Patients and Providers Act, proposing annual updates tied to the Medicare Economic Index—but legislative action remains uncertain.
Healthcare organizations that invest in analytics, provider education, automation, and oversight can turn denial management from a costly burden into a proactive strategic advantage. In 2025 and beyond, success depends on preventing denials before they happen, transforming what was once a reactive process into a powerful driver of financial sustainability.
Conclusion
The 2026 Medicare reimbursement squeeze is a fundamental inflection point for healthcare organizations. The combination of a 2.83% conversion factor reduction, 420 CPT code changes, rising denial rates, and higher operational costs creates unprecedented financial pressure.
But this isn’t a problem without solutions. Healthcare organizations that take proactive action—mastering CPT code changes, improving front-end accuracy, deploying intelligent claims scrubbing, optimizing denial management, and partnering with expert RCM services—can not only survive the Medicare squeeze but emerge stronger and more financially resilient.
The question isn’t whether your organization will feel the impact—it’s whether you’ll respond reactively or strategically.