In 2026, healthcare organizations are hiring aggressively to expand access, stabilize coverage, and support growth initiatives. On paper, provider capacity is increasing. In practice, many finance leaders are discovering that those investments are not converting into revenue on schedule.
The issue is not productivity, payer mix, or billing execution. It is credentialing.
When newly hired providers are not fully credentialed and enrolled with payers, they cannot bill for services rendered. Every day of delay directly translates into lost revenue, delayed cash inflows, and forecasting uncertainty. Recent industry research shows that more than half of hospitals and provider groups now report material financial losses caused specifically by provider credentialing delays, with many organizations losing over $1 million annually due to delayed enrollment and billing activation.
What was once treated as an administrative prerequisite has become a revenue velocity constraint— one that distorts cash flow, weakens forecasting accuracy, and erodes margins without triggering obvious alarms in traditional financial reporting.
Why Credentialing Delays Create a Forecasting Risk for CFOs
Credentialing delays do more than defer reimbursement. They undermine financial planning.
When a provider is hired, finance teams model expected revenue ramp based on clinic schedules, payer mix, and historical reimbursement. Those projections assume a predictable transition from clinical readiness to billing readiness. Credentialing breaks that assumption.
Industry data shows that credentialing and payer enrollment frequently take 90 to 120 days, even when providers are fully licensed and ready to see patients. During this period:
- Claims are either held, denied, or never submitted
- Cash inflows are deferred with no guaranteed recovery
For CFOs, this creates a blind spot. Staffing costs hit the P&L immediately, while revenue activation remains uncertain. The result is margin compression despite hiring — a paradox many finance teams are now facing across ambulatory groups, hospitals, and multi-specialty practices.
- Neolytix • MC & CVO
Medical Credentialing & CVO
Credentialing Delays Translate into Daily Revenue Leakage
The financial impact of credentialing delays is not abstract. It is measurable at the provider-day level.
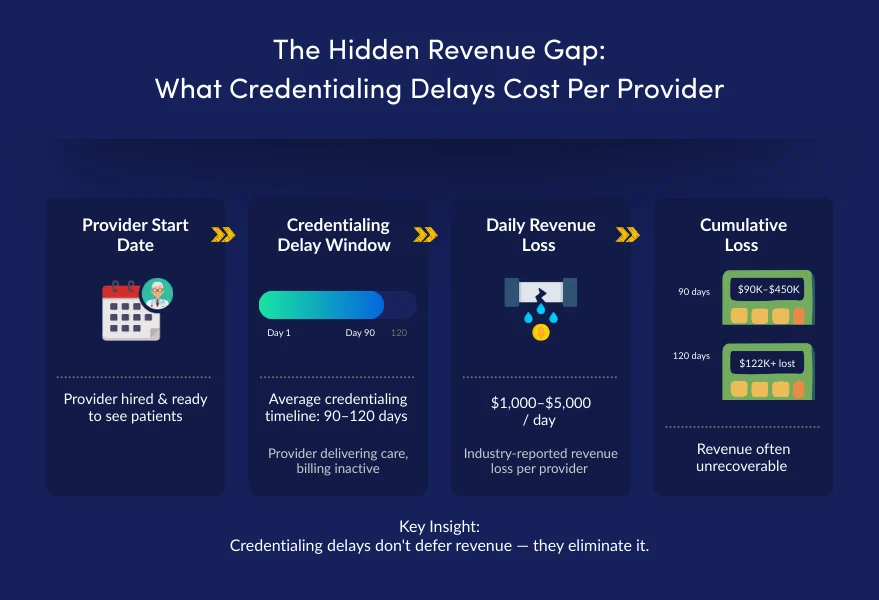
National surveys of provider groups and health systems indicate that organizations lose $1,000 to $5,000 per provider per day while enrollment remains incomplete. Over a standard 90-day delay, that equates to:
- $90,000–$450,000 in unrecoverable revenue per provider
- Six-figure losses before a single clean claim is submitted
Physician-specific analysis shows that a 120-day credentialing delay can result in approximately $122,000 in lost billable revenue per provider, depending on specialty and payer mix.
This is not deferred revenue — much of it is permanently lost. Retroactive billing is often restricted by payer policies, timely filing limits, and enrollment effective dates. Once those windows close, revenue leakage becomes irreversible.
Read more: Why US Provider Groups Are Turning to Credentialing Automation to Fix RCM Bottlenecks
Credentialing Impact on Revenue Cycle Performance Goes Beyond Billing Delays
While the inability to bill is the most visible consequence, the credentialing impact on revenue cycle performance extends much further downstream.
Denials and Rework Costs
When providers begin seeing patients before provider enrollment and credentialing are finalized, claims are frequently denied due to provider eligibility and enrollment status—not patient enrollment issues. Industry research shows that provider-related enrollment gaps contribute to a meaningful share of preventable claim denials, many of which are never appealed because of administrative effort, delayed resolution timelines, or low recovery probability. These denials add rework costs, delay reimbursement, and further extend days in accounts receivable, compounding revenue loss beyond the initial credentialing delay.
Each denied claim adds:
- Manual rework and follow-up
- Longer reimbursement timelines
- Increased days in A/R
- Higher write-off risk
Distorted Accounts Receivable Metrics
Delayed credentialing artificially inflates A/R metrics. Claims that could have been submitted cleanly are either held or denied, pushing receivables into aging buckets that do not reflect actual care delivery performance. This makes revenue cycle benchmarking misleading and obscures where operational efficiency actually breaks down.
Time-to-First-Claim as a Financial KPI
Increasingly, finance leaders are tracking time-to-first-claim—the period between provider start date and first successful claim submission. Longer time-to-first-claim correlates directly with delayed cash flow, weaker quarterly results, and reduced confidence in hiring ROI.
Credentialing is the dominant driver of that metric.

Why Healthcare Revenue Leakage Often Goes Unnoticed
One of the most dangerous aspects of credentialing delays is that the resulting healthcare revenue loss rarely appears as a single, obvious line item. Instead, it is dispersed across:
- Missed billing opportunities
- Denials written off as “administrative”
- Delayed cash collections
- Underperforming provider ramp curves
As a result, organizations often invest heavily in downstream RCM optimization—denials management, payer follow-up, coding accuracy—while overlooking one of the earliest and most expensive bottlenecks in the revenue lifecycle.
A 2026 industry report found that despite mounting financial losses, only a small percentage of healthcare organizations have invested in technology or process modernization specifically targeting credentialing workflows.
The Financial Impact Compounds Rapidly at Scale
For organizations onboarding providers continuously, the impact multiplies quickly. Consider a group hiring 10 providers annually:
- Average delay: 90 days
- Conservative daily loss: $2,000 per provider
- Annual revenue leakage: $1.8 million
This calculation excludes secondary costs such as denial management, staffing inefficiencies, and forecasting inaccuracies. At scale, credentialing delays quietly become one of the largest sources of preventable revenue loss in healthcare finance.
Conclusion: Credentialing Delays Revenue Loss Is a Cash Flow Risk — Not a Back-Office Issue
In 2026, credentialing delays revenue loss is more than an operational inconvenience. It is a cash flow and predictability risk that directly affects revenue activation, forecasting accuracy, and hiring ROI. Every day a provider cannot bill represents lost revenue that may never be recovered.
Leading organizations are responding by reframing credentialing as revenue infrastructure, not administrative overhead. That shift prioritizes:
- Visibility into credentialing and enrollment status before claims are submitted
- Alignment between credentialing, onboarding, and revenue cycle teams
- Standardized, trackable workflows across payers and locations
Platforms like InCredibly, our internal credentialing management platform support this approach by providing real-time visibility into credentialing status, enrollment progress, and risk exposure across multiple payers. When credentialing is managed as a financial control point rather than paperwork, staffing investments convert into billable revenue faster, with fewer downstream surprises.
- Neolytix • Contact Us
Contact Us
Neolytix partners with healthcare organizations across revenue cycle, credentialing, and administrative operations, 14+ years of expertise and AI-enabled automation to reduce inefficiencies and drive sustainable growth.
Frequently Asked Questions
Why can’t new providers bill insurance during credentialing?
Because payers require providers to be fully credentialed and enrolled before accepting claims. Services rendered before enrollment approval are typically denied or deemed non-billable.
How much revenue is lost due to provider credentialing delays?
Industry data shows losses ranging from $1,000 to $5,000 per provider per day, with six-figure losses common during 90–120 day delays.
Do credentialing delays impact the entire revenue cycle?
Yes. They drive claim denials, inflate A/R, delay cash flow, and distort financial forecasting across the revenue cycle.
What is time-to-first claim, and why does it matter financially?
Time-to-first-claim measures how quickly a new provider generates their first reimbursable claim. Longer timelines delay cash inflows and increase revenue leakage.
How can healthcare organizations reduce revenue loss from credentialing delays?
By prioritizing enrollment visibility, aligning credentialing timelines with hiring plans, and treating credentialing as a revenue-critical function rather than a purely administrative task.
Author
-
Merin Mary Thomas is a healthcare communications specialist with a background in Mass Communication and English Literature. She translates complex healthcare operations and innovations into clear, actionable insights, using storytelling to highlight best practices, industry trends, and strategies that help providers streamline workflows and enhance patient care.