Healthcare leaders are constantly balancing the need to control administrative costs with the imperative to protect revenue. Choosing a billing partner is rarely just about the lowest rate—what matters is the total impact on collections, cash flow, and internal resources. This guide provides a practical framework for evaluating revenue cycle management (RCM) vendors, so your cost-conscious decisions also protect your bottom line.
Understanding Total Cost Beyond the Rate Card
Many organizations initially evaluate vendors based on hourly rates, per-claim fees, or overall contract cost. While cost is important, focusing only on rates can obscure the true economics of billing:
- Revenue leakage: Even small gaps in collections add up over time.
- Cash flow delays: Slower accounts receivable (AR) cycles increase dependence on working capital.
- Internal burden: Rework caused by incomplete documentation, payer denials, or unresolved claims pulls staff away from higher-value tasks.
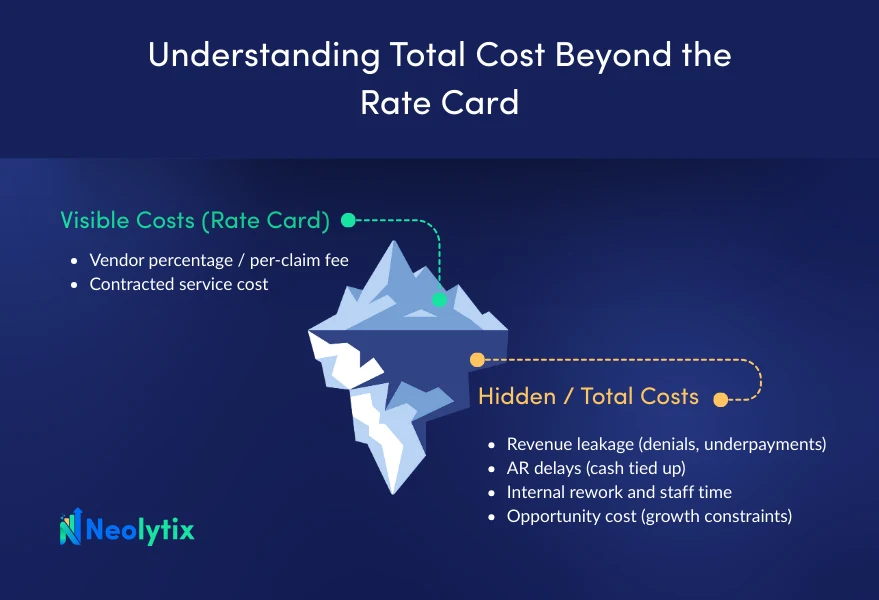
These costs are rarely visible on invoices, but they affect financial performance more than minor differences in service fees.
Example Scenarios
- Solo/Small Practice: A 2-physician family practice collects $1.2M annually. A 1.5% loss from preventable denials = $18,000/year. Choosing a vendor charging 5% ($60K) versus a more capable vendor at 6% ($72K) results in $12K higher fees, but the net cost is only $6K after recaptured revenue—before factoring in time physicians spend chasing issues.
- Mid-Market Practice: A 15-provider specialty group collects $12M annually. A 2% denial gap = $240,000 left uncollected. Add 15 extra days in AR and the practice finances $500K+ in unnecessary working capital—roughly the cost of one additional provider they could hire.
- Cash Flow Impact: Every 10 days of extended AR on $10M annual revenue ties up roughly $274K in receivables. At current interest rates, this equals $15-20K in opportunity or carrying cost annually.
These examples illustrate that “cheaper” rates don’t automatically mean lower total cost. Understanding total cost requires evaluating vendor performance, process integration, and adaptability.
Read More: The $2M Revenue Leak: Critical KPIs Most Healthcare Organizations Completely Ignore
Key Questions to Ask When Evaluating Vendors
Instead of relying on generic descriptors like “high-performance” or “efficient,” ask vendors specific questions to uncover true capabilities:
Revenue Controls & Leakage Prevention
- What revenue controls or audits do you have to prevent revenue leakage?
- How do you identify and flag underpayments before they age out?
- What percentage of claims do you review for charge capture accuracy?
Denial Resolution Quality
- How do you measure whether your team is actually resolving denials versus just resubmitting them?
- Do you track denial resolution by root cause or only by volume?
- Technical Insight: Some vendors submit incorrect resolutions that reset the payer clock. The claim appears “worked,” but the underlying issue is unresolved—simply delayed 30-45 days.
Clean Claims Rate Accuracy
- How do you calculate clean claims rate?
- Technical Insight: Many EMRs generate a new claim number for each submission. A claim denied twice and paid on the third attempt may appear as three separate “clean” claims. Ask vendors how they track first-pass resolution tied to the original Date of Service.
- What is your first-pass acceptance rate by payer?
Accountability & Transparency
- Can you show aged AR by bucket with actual claim-level detail?
- What is the escalation path for claims stuck beyond 60 days?
- How do you report on trends proactively, not just on request?
Red Flags to Watch For
- Vendors who only report claims submitted, not claims paid.
- Vendors unable to segment denial data by root cause.
- Vendors reluctant to provide claim-level AR aging reports.
- Lack of clear escalation procedures or governance.
These warning signs often indicate structural limitations rather than isolated errors. Early identification helps avoid downstream complications.
Structuring a Vendor Evaluation for Cost-Effectiveness
- Combine cost with performance metrics: Compare service fees alongside historical AR velocity, denial resolution rates, and revenue capture.
- Prioritize expertise for complexity: Practices with multiple specialties or frequent payer changes benefit from vendors who excel in handling variable scenarios.
- Check integration and communication: Vendors that collaborate with coding, clinical, and access teams reduce preventable errors.
- Use questions as a checklist: Ask about revenue controls, denial resolution, clean claim tracking, and transparency to assess the real cost of a vendor relationship.
Conclusion: Smarter Decisions Protect Revenue
The most important question for healthcare leaders isn’t simply “How much does billing cost?” but “What does poor billing cost us?” Use these questions and evaluation criteria to uncover the total economic impact of a vendor, beyond the rate card. By combining cost discipline with operational insight, organizations can select RCM partners that preserve revenue, accelerate cash flow, and reduce internal burden—while still respecting budget constraints.
Read More: AI-Driven RCM: The Future of Revenue Cycle Management in Healthcare