Every healthcare organization knows that credentialing takes time. What many don’t fully account for is how much that time actually costs—in delayed revenue, disrupted cash flow, and stalled strategic planning.
Provider credentialing is not just an administrative checkbox. It is a revenue recognition event. And when the provider credentialing timeline stretches unpredictably from 60 to 180 days, the financial and operational consequences reach far beyond the credentialing team. For CFOs and financial planners, this uncertainty creates material planning gaps that affect quarterly projections, cash flow management, and strategic hiring decisions

What Is Provider Credentialing?
Provider credentialing is the formal process of verifying a healthcare provider’s qualifications. This includes education, licensure, training history, board certifications, and past work experience. No provider can see patients or submit insurance claims until this process is complete.
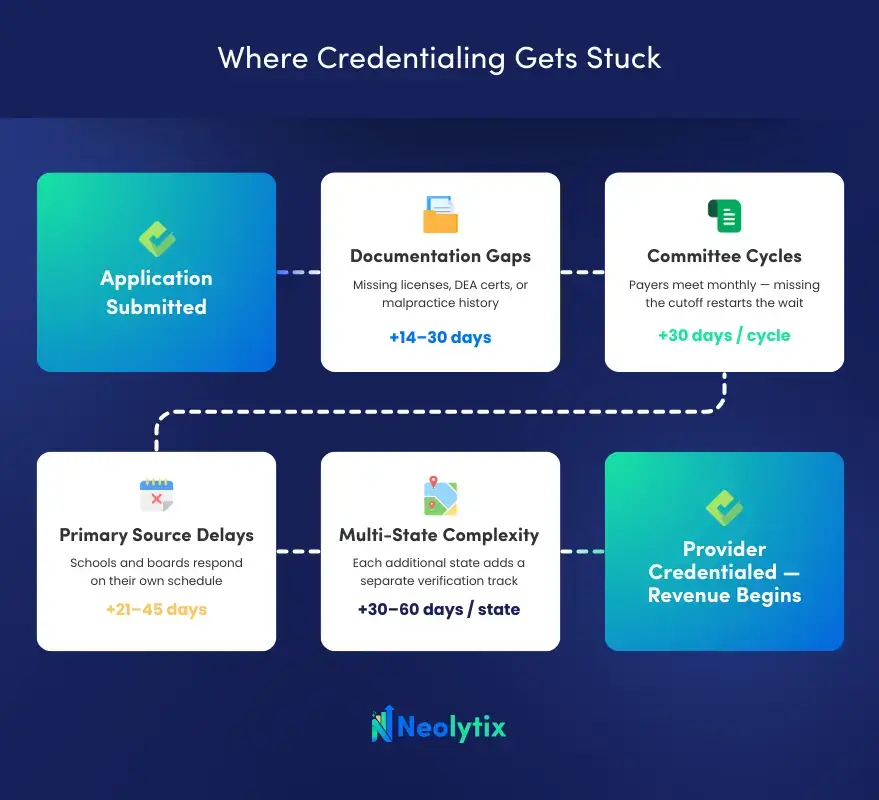
Provider Credentialing Timeline: What Happens at Each Stage
| Stage | Typical Timeframe | What’s Actually Happening |
| Document Collection & Application Prep | 1–2 weeks | The credentialing team gathers licensure, education records, board certifications, work history, and malpractice coverage. Gaps or inconsistencies here are the #1 cause of downstream delays. |
| Application Submission to Payers | 1–2 weeks | Completed applications go out to each payer separately—each with its own form, format, and requirements. Multi-payer submissions multiply this effort significantly. |
| Primary Source Verification | 4–6 weeks | Payers independently confirm credentials with medical schools, licensing boards, and previous employers. This step depends entirely on third-party response times—outside anyone’s direct control. |
| Payer Internal Review | 4–8 weeks | The payer’s internal team reviews the application for compliance, runs background checks, and prepares the file for committee presentation. Volume backlogs and seasonal hiring surges affect this window. |
| Credentialing Committee Approval | 1–2 weeks | A formal committee reviews and votes on the application. Most committees meet monthly—missing a cycle means waiting for the next one. |
| Contracting & Network Enrollment | 2–4 weeks | Once approved, contracts are issued, reviewed, negotiated if needed, and signed. The provider is officially enrolled and billing can begin. |
| Total Timeline | 90–180 days | Varies based on payer type, state, specialty, and application quality. Commercial payers average 90–120 days. Multi-state credentialing or complex backgrounds can reach 180 days or beyond. |
The 5 Key Steps in the Provider Credentialing Process
Understanding what actually happens during credentialing helps explain why timelines vary—and where delays tend to hide.
- Application Submission Every provider must submit a detailed application covering their education, employment history, hospital privileges, and malpractice coverage history. Completeness matters here more than speed. An incomplete or inconsistent application will stall at the next stage—sometimes for weeks.
- Supporting Documentation Along with the application, providers must supply a specific set of documents. This includes their DEA registration number, active medical license, board certification status, malpractice carrier details, and any required health documentation. Each payer may have a slightly different list. Missing a single item can trigger a correction request and reset the clock.
- Primary Source Verification This is where external timelines take over. The payer—or a credentials verification organization—contacts medical schools, state licensing boards, and previous employers directly to confirm every credential on the application. No shortcuts exist here. Verification moves at the pace of the third parties being contacted.
- Approval and Network Enrollment Once verification is complete, the application goes to a credentialing committee for review and approval. After approval, a participation contract is issued and executed. Only at this point can the provider begin billing for services and receiving reimbursement from that payer.
- Recredentialing Credentialing is not a one-time event. Most payers require providers to recredential every two to three years. This process re-verifies licensure, updates malpractice history, and reflects any changes in clinical privileges or additional training. Organizations that manage this proactively avoid lapses that can temporarily suspend billing rights—an easily preventable but surprisingly common revenue disruption.
Key Factors and Challenges That Delay the Provider Credentialing Process
Most people assume credentialing delays come from one source—the payer. The reality is more layered.
Incomplete or inconsistent documentation is one of the most common causes of delay. If any piece of a provider’s application conflicts with primary source records, the payer flags it and requests corrections. Each correction cycle can be added in weeks. In some cases, it pushes the application to the next committee meeting cycle, extending the timeline by a month or more.
Primary source verification adds time by design. Every credential must be confirmed at its original source. Medical schools, state licensing boards, specialty certification bodies—each operates on its own schedule. Healthcare organizations have no control over how quickly those third parties respond.
Payer-specific committee schedules create another layer of unpredictability. Commercial payers convene credentialing committees on fixed schedules—monthly, in many cases. A provider whose application arrives the day after a committee meets waits a full month before review begins.
Multi-payer complexity compounds the problem. Most healthcare organizations contract multiple payers. A provider might receive Medicare approval in six weeks but wait four additional months for a major commercial carrier. Until all relevant payers approve, the provider cannot serve a full patient panel.
State licensing timelines vary significantly. In Texas, for example, the credentialing process can extend to 180 days due to state-specific regulatory requirements. Providers credentialing in multiple states face compounding delays.
None of these factors show up in a standard status update that reads “application in review.”
Want to understand what these delays actually cost your organization? Read our in-depth breakdown of how credentialing delays translate into revenue loss and cash flow risk:
How Healthcare Organizations Can Reduce Credentialing Delays and Improve Revenue Predictability
The good news is that most credentialing delays are not inevitable. Many stem from controllable factors—and organizations that address them proactively see meaningfully shorter timelines and more reliable revenue forecasting.
Build payer-specific completion benchmarks. Historical credentialing data is one of the most underused planning tools available. Medicare enrollment for a psychiatrist in Ohio follows different patterns than commercial payer approval for a hospitalist in California. Tracking actual completion times by payer, state, and specialty over time allows organizations to replace guesswork with specific, evidence-based forecasts.
Review applications for risk before submission. Incomplete documentation, conflicting employment history, and missing attestations are among the most common delay triggers—and all are identifiable before an application ever reaches a payer. A structured pre-submission review catches these issues early, preventing the correction cycles that push applications past committee deadlines and add weeks to timelines.
Connect credentialing milestones to financial planning. When credentialing operations and finance teams work from the same projected completion dates, CFOs can build quarterly revenue projections on actual data rather than broad assumptions. This requires treating credentialing not as a back-office administrative function, but as a direct input to revenue recognition planning.
Together, these shifts move credentialing from a reactive process—one that reports on what has happened—to a predictive operation that informs what leadership can plan for. That distinction has measurable financial value, particularly for healthcare organizations managing multiple provider pipelines simultaneously.
How InCredibly Transforms Status Tracking Into Revenue Forecasting
Organizations need more than faster credentialing—they need predictable credentialing that supports financial planning. InCredibly delivers this through four fundamental capabilities.
Historical performance data across payer-state-specialty combinations replaces generic timeline estimates with specific benchmarks. Medicare credentialing for psychiatrists in Texas versus California shows measurable differences. Commercial payer processing for orthopedic surgeons versus primary care physicians follows distinct patterns. InCredibly captures these patterns to build accurate completion forecasts.
Predictive timelines based on actual completion patterns enable CFO conversations with specific dates rather than vague quarters. Instead of “somewhere in Q2,” finance teams receive “billing capability by April 18” with confidence levels based on historical performance. This transforms credentialing from administrative uncertainty into revenue recognition planning.
Risk-flagging for applications likely to experience delays enables proactive intervention before timelines slip. Incomplete documentation, conflicting work history, missing attestations trigger alerts when applications enter the system. Teams address completion risks immediately rather than discovering problems during payer review cycles.
Proactive milestone management versus reactive status checking shifts credentialing from tracking what happened to managing what needs to happen next. Automated workflows identify when applications approach projected milestones without expected progression. Intervention occurs before delays affect revenue recognition dates finance incorporated into quarterly projections.
This approach delivers measurable financial impact. Earlier, more accurate revenue forecasting enables confident quarterly guidance. Reduced buffer time in hiring decisions accelerates provider recruitment timelines. Data-driven conversations with payers about processing delays create accountability. Benchmarking against actual completion times replaces assumptions with evidence.
Frequently Asked Questions
How long does the provider credentialing timeline typically take?
The provider credentialing timeline ranges from 60 to 180 days, depending on payer type, provider specialty, state requirements, and application completeness. Commercial payer enrollment averages 90 to 120 days. Medicare through PECOS typically takes 60 to 90 days. Multi-state credentialing or complex provider backgrounds can push timelines to six months or beyond.
What causes delays in the provider credentialing process?
Common causes include incomplete or inconsistent documentation, slow primary source verification from third parties such as medical schools and licensing boards, payer credentialing committee schedules, and multi-payer coordination complexity. Each delay source compounds the others, extending overall timelines in ways that standard status updates do not reflect.
How does a credentialing delay affect healthcare organization revenue?
Every week a provider cannot bill represents direct revenue loss. For a provider with a $25,000 monthly revenue expectation, a two-month delay equals $50,000 in unrealized revenue. At the organizational level, these losses affect quarterly performance, cash flow planning, and the ROI of recruitment investments.
Why doesn't status tracking solve the credentialing timeline problem?
Status updates show activity—not completion forecasts. A status marked “in review” on day 20 looks identical to the same status on day 80. Finance teams cannot build reliable revenue projections from activity logs. They need payer-specific completion estimates tied to historical performance data.
What information should CFOs request from their credentialing teams?
CFOs should ask for average days-to-first-bill by payer and specialty, projected revenue recognition dates by provider, the percentage of each provider’s patient panel billable in each month, and any applications flagged as at-risk for delay. These metrics connect credentialing operations directly to financial planning.
Can outsourcing credentialing improve timeline predictability?
Yes. Experienced credentialing partners bring historical payer performance data, established follow-up protocols, and pre-submission risk review processes. These capabilities reduce both average timeline length and the variance between projected and actual completion—improving the reliability of revenue forecasts.






