Understanding Total Cost Beyond the Rate Card
Medical billing remains surprisingly common among healthcare organizations (HCOs). But in 2025, relying on paper, fax, spreadsheets, or non-integrated systems is no longer just outdated — it’s costly. Organizations using manual workflows face:
- Higher claim denial rates
- Longer reimbursement cycles
- Increased administrative burden
- Costly error corrections
- Greater compliance risk
Industry data highlights the scale of the problem:
- Billing error rates for U.S. healthcare claims are around 7 – 10 %, with errors contributing to costly denials and rework.
- Manual billing errors can cost practices 10–15 % of potential revenue annually.
- Errors in billing contribute to administrative expenses equivalent to billions of dollars across the U.S. system each year.
- Claim denials cause delays of up to 30 days or more vs. clean claims.

Medical billing errors alone cost U.S. providers over $2.5 billion annually, and inaccurate billing or charge capture can lead to a 3–5% net revenue loss. The shift toward modern billing services is accelerating because healthcare leaders recognize that inefficiencies hidden in manual processes quietly erode their bottom line.
Why Manual Billing Workflows Fail
Consider a mid-sized clinic still mailing paper bills, entering codes manually, and tracking claims in spreadsheets. On the surface, it may appear manageable — but every step introduces risk:
Revenue Controls & Leakage Prevention
- Data entry mistakes — Mistyped patient info, missing fields, or incorrect insurance details
- Coding inconsistencies — Higher risk of outdated, mismatched, or incomplete codes
- Slow submissions — mailing, printing, or faxing dramatically slows down revenue
- Missed follow-ups — Lost claims and unappealed denials
- Administrative overload — Staff spend hours on tasks automated systems handle instantly
Even a single mistake can trigger a cascade of delays, rework, and lost revenue. Manual workflows also lack transparency — leaders cannot track claims in real time, which allows problems to compound.
Outdated billing processes are a major driver of revenue leakage in U.S. healthcare.
Why Outsourcing Is Surging: The Shift to Tech-Enabled Medical Billing Services
The U.S. medical billing outsourcing market reached $5.9 billion in 2024 and is predicted to reach 16.9 billion by 2033. The drivers are clear:
- Staff shortages: Revenue cycle staff turnover is at an all-time high
- Rising payer scrutiny: More documentation, more rejections, more rules
- Higher compliance pressure: HIPAA, payer audits, interoperability rules
- Automation demands: AI-assisted coding, claim scrubbing, and digital workflows
- Need for predictable cash flow: Manual systems can’t deliver consistency
Modern medical billing outsourcing is not just about reducing workload — it’s about protecting revenue and accelerating collections.
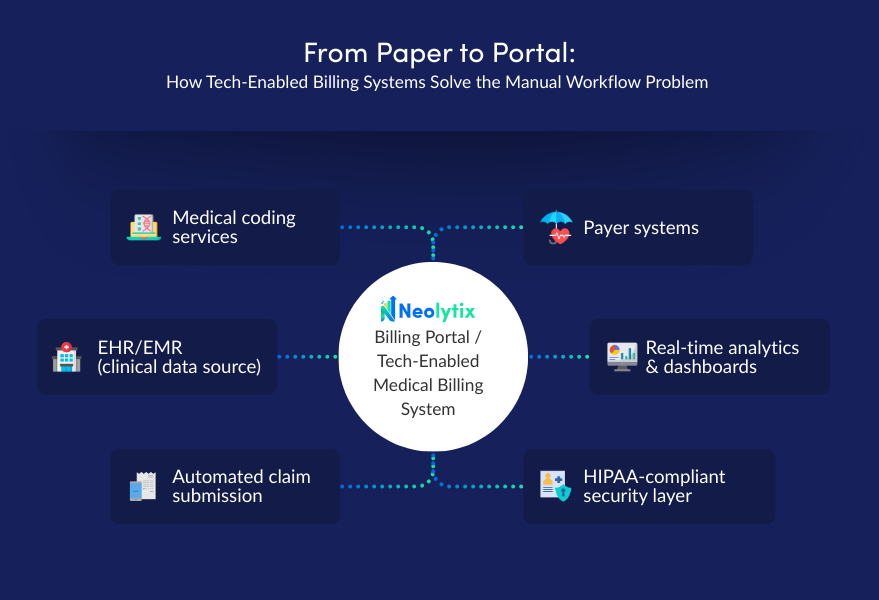
From Paper to Portal: How Tech-Enabled Billing Systems Solve the Manual Workflow Problem
Neolytix provides a modern, technology-driven billing model that combines automation, accuracy, and real-time visibility. Here’s how:
1. EHR/EMR Integration for Clean Data Flow
Seamless, real-time data exchange between clinical and billing systems reduces manual entry, ensures accurate claims, and minimizes patient or charge data mismatches.
2. Automated Claim Submission & Error-Free Billing
AI-driven automation minimizes errors and accelerates reimbursement cycles, reducing manual workload and human coding mistakes.
3. Real-Time Tracking & Analytics
Custom dashboards and EMR-integrated reporting provide full transparency into claim status, denial trends, and A/R aging for better financial oversight.
4. HIPAA-Compliant, Secure Infrastructure
Secure, HIPAA compliant billing workflows protect sensitive patient and payer data while ensuring audit readiness.
5. Lower Administrative Burden & Reduced Cost
Secure, HIPAA compliant billing workflows protect sensitive patient and payer data while ensuring audit readiness.
Who Benefits Most from Portal-Based Billing?
- Small to Mid-Sized Organizations: Lean teams gain reduced staffing pressure, fewer errors, and faster claim processing.
- Large Hospitals & Multi-Provider Networks: Scalable workflows maintain consistency across departments and multiple EHRs.
- Specialty Clinics (Mental Health, Dental, Therapy, Primary Care): Complex coding requirements are managed efficiently, reducing denials.
- New Healthcare Organizations: Implementing automated billing from day one avoids the pitfalls of manual workflows.
The Bottom Line: Manual Billing Is a Financial Liability
Manual workflows are no longer just inefficient — they actively harm financial performance. Errors, delays, and lack of transparency increase denials and reduce cash flow.
Automated billing systems, integrated EHR workflows, and professional medical billing outsourcing offer a clear path to:
- Faster collections
- Fewer errors
- Stronger compliance
- Predictable revenue
Moving from manual billing to portal isn’t just an upgrade — it’s a strategic financial move
Frequently Asked Questions
What are medical billing services, and why are they critical in 2026?
Medical billing services manage claim submission, follow-ups, and reimbursements. In 2026, they are critical because manual billing increases denials, delays payments, and creates compliance risk. Automated, portal-based medical billing services improve accuracy, speed collections, and protect revenue.
How do manual billing workflows lead to revenue loss?
Manual billing causes revenue loss through data entry errors, delayed submissions, missed payer follow-ups, and limited claim visibility. These issues increase denial rates, extend reimbursement timelines, and reduce overall cash flow.
What is medical billing outsourcing, and how does it help in 2026?
Medical billing outsourcing shifts billing operations to specialized healthcare billing service providers using automation and expert teams. In 2026, outsourcing helps organizations address staffing shortages, reduce denials, and maintain consistent revenue cycle performance.
Are portal-based medical billing services HIPAA compliant?
Yes. Modern portal-based medical billing services are built to be HIPAA-compliant, using secure infrastructure, controlled access, and encrypted data exchange to protect patient and payer information and support audit readiness.
How does EHR-integrated billing reduce claim denials?
What role do medical coding services play in billing accuracy?
Medical coding services ensure accurate ICD-10, CPT, and HCPCS coding. Proper coding reduces denials, prevents revenue leakage, and supports compliance with payer and regulatory requirements.
Is moving from manual billing to portal-based billing worth it in 2026?
For most U.S. healthcare organizations, moving to portal-based billing in 2026 is a strategic investment. Reduced errors, faster payments, and stronger compliance typically outweigh the cost of modern medical billing services.