Payer Enrollment Services
While you’re drowning in payer paperwork, your competitors are seeing patients. Let’s fix that.
Every day your providers sit on the enrollment sidelines costs you real money – about $8,000 per provider, per day. That’s not just lost revenue; that’s salaries paid without patient care, frustrated physicians threatening to leave, and your CFO’s increasingly concerned emails.
At Neolytix, we turn the 120-day enrollment marathon into a 45-day sprint. Our AI-powered Incredibly workflow platform and expert team have enrolled over 5,000 providers across all 50 states. We speak fluent PECOS, dance with CAQH daily, and know exactly which payer rep to call when applications mysteriously “disappear.”
The Real Cost of Enrollment Delays (And Why Your Current Process Isn't Working)
Your Enrollment Nightmare, By the Numbers
Dr. Sarah Chen, your new star cardiologist, started three weeks ago. She’s eager, patients love her, but she can’t bill a single insurance claim. Sound familiar? Here’s what’s really happening while you wait:
- $240,000 – Average revenue lost per provider during typical 90-day enrollment
- 73% of applications have errors causing 30-60 day delays
- 42% of new providers consider leaving during enrollment delays
- 18 hours – Average weekly time your staff spends on enrollment follow-ups
The Hidden Costs Nobody Talks About:
- Patient abandonment: “Sorry, we don’t take your insurance yet” leads to lost patients forever
- Staff burnout: Your team playing phone tag with payers instead of supporting providers
- Compliance risks: One missed revalidation = potential Medicare exclusion
- Cash flow chaos: Retroactive billing nightmares and A/R headaches
But here’s the kicker: Most practices think this is just “how enrollment works.” It doesn’t have to be.


Transform Provider Enrollment from Your Biggest Bottleneck to Your Competitive Advantage
Welcome to Enrollment That Actually Works (Yes, Really)
Forget everything you know about provider enrollment. No more:
- Faxing the same documents 17 times
- Playing “guess the rejection reason” with payers
- Discovering your CAQH expired… yesterday
- Praying to the enrollment gods for Medicare approval
The Neolytix Difference: Where AI Meets "We've Done This 5,000 Times"
Our provider enrollment services combine:
Incredibly AI Workflow Platform
- Auto-populate applications with 99% accuracy
- Up to date payer requirements
- Cockpit view of Providers & Payers so you stay in control
- Automated follow-up sequences that actually work
Human Expertise That Matters
- Dedicated enrollment specialists
- Direct payer relationships built over 13+ years
- Former payer-side pros who know the inside tricks
- Proactive monitoring of your enrollment pipeline
Complete Transparency
- Live dashboard showing every application status
- Weekly executive summaries you’ll actually read
- Proactive alerts before problems happen
- ROI reporting that makes your CFO smile
Why Choose Neolytix for Physician Credentialing Services?
Our credentialing services for hospitals, groups, IPAs, and healthcare organizations ensure that providers are fully compliant with industry standards, streamlining the process for both new and existing staff members.
Measurable Business Impact:
Step 1: The 48-Hour Sprint Start
Within 2 days of signing, we:
- Audit your current enrollment mess (diplomatically)
- Identify quick wins and priority payers
- Create your custom enrollment roadmap
- Assign your dedicated enrollment dream team
Step 2: The Document Blitz
Our AI-powered system:
- Custom AI Agents that can extracts data from existing files
- Identifies missing documents
- Creates a single source of truth
- Pre-validates everything against current payer requirements
Step 3: The Application Assault
This is where the magic happens:
- Custom AI Agents that can extracts data from existing files
- Identifies missing documents
- Creates a single source of truth
- Pre-validates everything against current payer requirements
Step 4: The Follow-Up Force
While others wait and hope:
- Automated follow-ups
- Direct payer portal access for real-time updates
- Escalation protocols for stuck applications
- Weekly status calls with your team
Step 5: The Victory Lap
Getting you operational fast:
- Immediate notification of approvals
- EFT/ERA setup for instant payments
- Complete handoff documentation Ongoing
- maintenance to prevent lapses
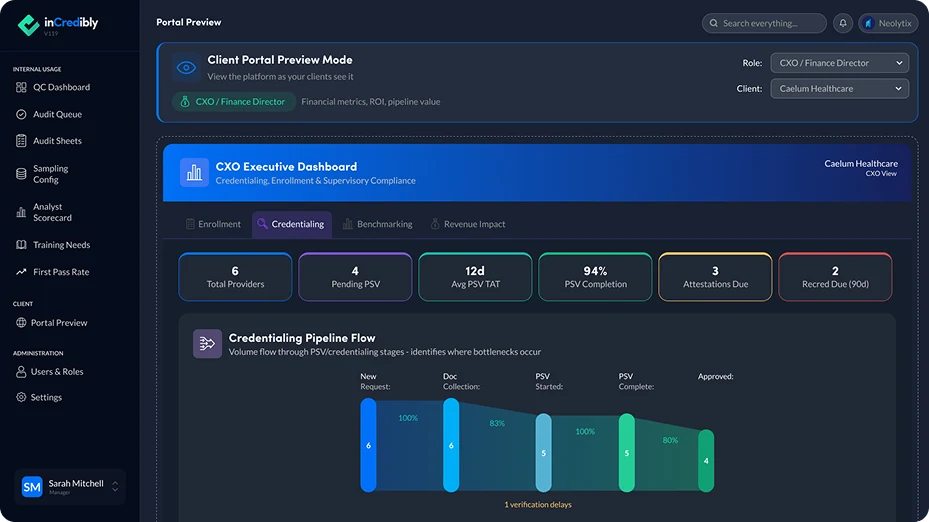
Incredible Credentialing. Revenue That Doesn't Wait.
inCredibly™ is Neolytix’s purpose-built provider data intelligence platform, built to turn provider enrollment from an administrative holding pattern into a forecastable revenue pipeline.
Most enrollment tools tell you where an application is. inCredibly tells you when the provider will start billing and exactly how much revenue is at stake while you wait.
What inCredibly brings to your organization:
- Sankey Pipeline Visualization — identifies revenue-blocking bottlenecks across all active payer workflows
- Payer Intelligence Engine — verified submission contacts, current requirements, and process nuances updated daily
- Smart Data Extraction — pulls provider information from NPPES, state boards, and existing documentation automatically
- Time Allocation Analytics — shows where 40–60% of analyst effort is lost to avoidable follow-up
- Stakeholder Dashboards — COO, Recruiter, and MSO views with role-specific reporting

Stop the Enrollment Madness - Your Providers (and CFO) Will Thank You
What You Get With Neolytix:
Faster Revenue Generation
- Start billing 50 days sooner on average
- Reduce revenue leakage from enrollment delays
- Accelerate ROI on new provider investments

Operational Excellence
- Free your staff for patient-facing activities
- Eliminate enrollment-related provider frustration
- Standardize processes across all locations

Complete Peace of Mind
- Never miss a revalidation deadline again
- Stay compliant with all payer requirements
- Sleep knowing experts handle your enrollment

Transparent Reporting
- Real-time visibility into every application
- Executive dashboards that actually make sense
- ROI metrics that justify the investment


The Bottom Line: Every Day You Wait Costs Money
While you’ve read this page, the average practice has lost $3,000 in delayed reimbursements. Your new providers are getting frustrated. Your staff is drowning in paperwork. But it doesn’t have to be this way.
Here’s What Happens Next:
- Free Enrollment Audit – We’ll analyze your current process and show you exactly where you’re losing time and money (spoiler: it’s probably worse than you think)
- Custom Fast-Track Plan – Get a detailed roadmap showing how we’ll cut your enrollment time by 50% or more
Get in touch with us
FAQs (The Questions You're Already Thinking)
How do you handle both credentialing AND enrollment simultaneously?
Our integrated approach treats credentialing and enrollment as complementary processes, not sequential ones. We submit enrollment applications as soon as primary source verification is complete, cutting total time-to-revenue by 45-60 days.
What if we have providers stuck in credentialing limbo right now?
We specialize in credentialing rescue operations. Our team will assess stuck applications, identify roadblocks, and implement recovery protocols. Most “impossible” cases just need expert intervention and direct payer relationships.
What about ongoing maintenance and revalidation?
That’s where we truly shine. Our platform automatically tracks all renewal dates, sends advance warnings, and manages the entire revalidation process. You’ll never miss a deadline or face a compliance lapse again.
Can your platform integrate with our existing systems?
inCredibly™ is built for integration. We connect with major practice management systems, EHRs, and credentialing databases. Our technical team handles all integration work—no IT burden on your side.
Ready to Turn Provider Enrollment from a Nightmare into a Competitive Advantage?
Your providers want to practice medicine, not chase paperwork. Your CFO wants revenue flowing, not excuses. You want a partner who gets it done. That’s exactly what we do.



